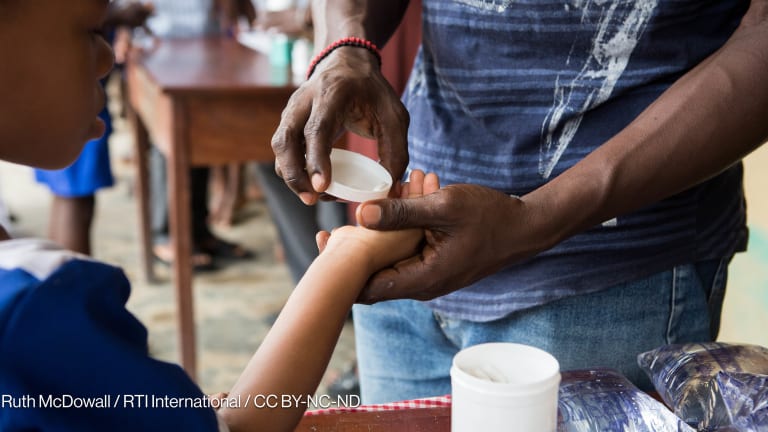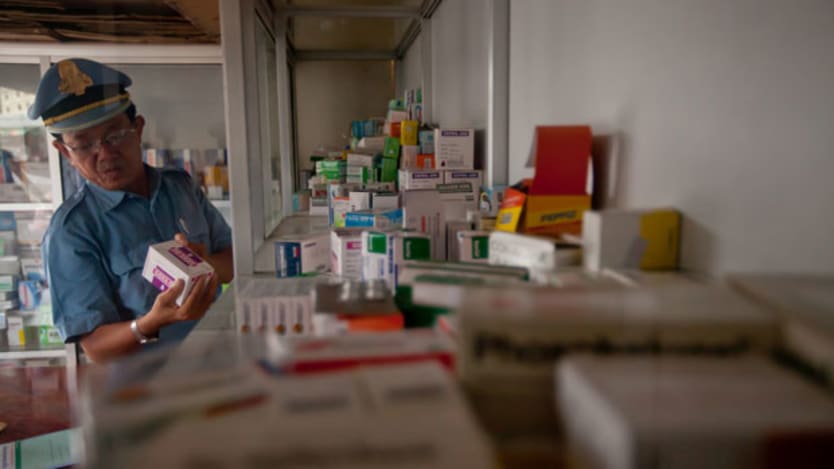
Lindsey Graham stood at a podium at the festooned Knight Conference Center in Washington’s Newseum in early December and addressed a room full of public health advocates, researchers and politicians gathered for the 2014 Malaria Champions Breakfast.
The gathering, organized by the nonprofit organization Malaria No More, was designed to recognize prominent allies in the fight to eradicate the mosquito-borne disease.
Graham, the Republican senator from South Carolina, is highly regarded within the malaria community for his staunch support of U.S. foreign assistance. His voice in Congress is one reason why the United States remains the largest funder of anti-malaria programs today.
As other speakers touted impressive progress in the global fight against malaria, though, it soon became clear Graham wasn’t interested in lingering on past accomplishments.
He had a more pressing message: U.S. funding for malaria is at risk.
“Look at the lives saved and the infrastructure that’s been developed in the last ten years,” said Graham, who is known for not mincing words. “All of that’s at risk. You’ll be pulling back at a time when you’re just about to get over the finish line.”
Over the past decade or so, the fight against malaria has gained momentum. Mortality dropped 47 percent between 2000 and 2013, according to the World Health Organization; the total number of infections in Africa fell from 173 million to 128 million — a 26 percent reduction that is largely the result of increased prevention and control measures. An estimated 584,000 people died of malaria in 2013.
Advocates see an opportunity to zero in on global eradication. Yet new drug resistance and looming funding cuts threaten to present an insurmountable cliff.
If the U.S. Congress is unable to relieve cuts on the discretionary budget in 2015, Graham cautioned, it will “pull the rug out” from small villages most vulnerable to malaria.
“I need your help in 2015,” Graham said. “2015 is the year to find a way to implement cuts that will not put children at risk who have the best chance of defeating malaria in our lifetime.”
Two steps forward
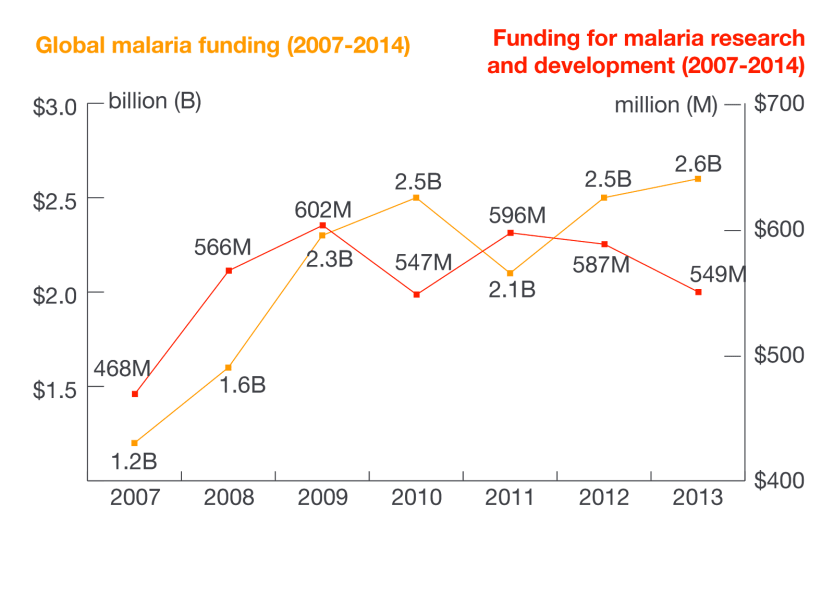
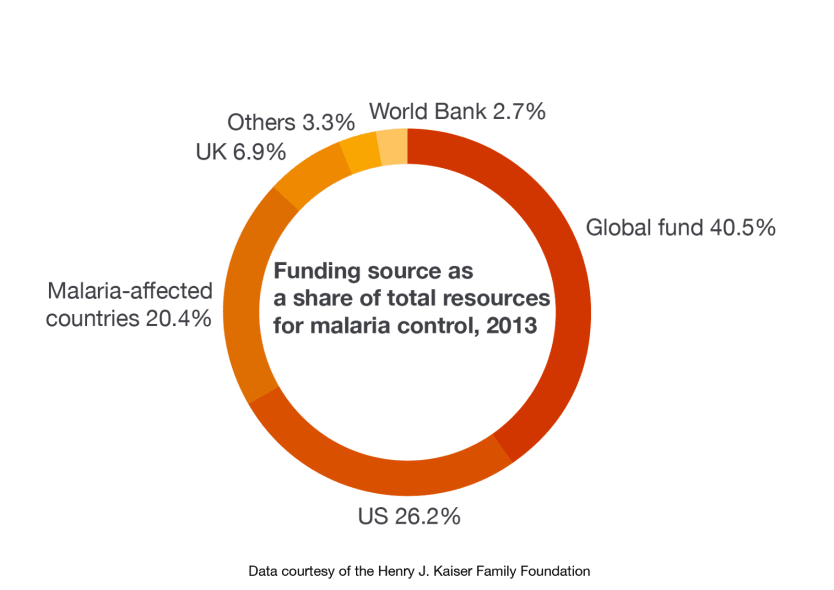
Global spending on malaria control totaled $2.6 billion in 2013, according to the Kaiser Family Foundation. Major funders include countries affected by the disease as well as the United Kingdom and the World Bank.
With 26 percent, though, the U.S. government is by far the largest funder of anti-malaria efforts; it’s also the single largest donor to the Global Fund to Fight AIDS, Tuberculosis and Malaria, which provides half of all anti-malaria funding worldwide.
U.S. bilateral funding for malaria is projected to increase to $701 million in 2015 — a $26 million increase from 2013.
Since its inception in 2002, the Global Fund has disbursed more than $7.1 billion in grant funding for malaria, and an approximate $1 billion of additional grant money has been signed, although not yet disbursed. It has allocated approximately $4.3 billion for malaria for 2014-2016, according to the Kaiser Family Foundation.
If the U.S. government is unable to find solutions to it’s discretionary budget woes, Graham warns, malaria funding in 2016 and beyond may plummet, leaving malaria-endemic countries without sufficient resources to cope.
“Any concerns about cuts to [the U.S. President’s Malaria Initiative] or to the Global Fund are real,” Scott Filler, the Global Fund’s senior disease coordinator for malaria, told Devex, emphasising the U.S. government’s critical role in combatting the parasite.
Funding for malaria research and development is already on a downward slope: It decreased by $38 million between 2012 and 2013 — the second consecutive year of declining R&D funds, according to the Kaiser Family Foundation.
Speaking after Graham during December’s Malaria Champions Breakfast, Mark Dybul, the Global Fund’s executive director, acknowledged that if bilateral and multilateral resources aren’t maintained, efforts to eliminate malaria are going to “start falling apart.”
“We’ll lose the game,” Dybul cautioned.
If Congress can’t sustain funding for malaria beyond 2015, a world free of the disease will likely elude mankind’s grasp once again.
New year, new agenda
Among all the development campaigns spawned by 2000’s U.N. Millennium Declaration, the global fight against malaria has been one of the most successful. Malaria incidence has been reversed; 55 countries are on track to meet the World Health Assembly and Roll Back Malaria Partnership target of reducing malaria incidence 75 percent by 2015 over 2000 levels.
But all that progress could unravel if the success of anti-malaria efforts leads to complacency and the disease slips on the list of priorities — which is what some anti-malaria activists fear is happening.
In September, on the fringes of the U.N. General Assembly, world leaders are expected to sign a global framework for post-2015 development. A recent draft listed health as one of 17 goals. Given other burgeoning health emergencies and the strong progress on malaria, many public health advocates worry that malaria will seem less urgent to policy-makers.
“Suddenly, the focus that malaria had is being very much diluted by the work that’s going on at the U.N.,” Jon Pender, vice president of government affairs at GlaxoSmithKline, told Devex.
What will it take?
It’s tough to put an end date or dollar amount on one of humanity’s oldest diseases. Roll Back Malaria’s Global Malaria Action Plan estimates the cost of ridding the planet of malaria at about $5.1 billion per year until 2020. Some experts disagree.
“If anyone could give you a detailed breakdown of the costs for the next 35 years, they’re lying to you,” said Alan Magill, director of the Bill & Melinda Gates Foundation’s Global Health Program. “Because what’s happening is more complicated, and it’s going to be very flexible and adaptive.”
Trouble is, for an estimate to be accurate, Magill explained, it must assume that today’s drugs, repellents and insecticides will remain effective.
But malaria’s drug resistance is growing; chemical interventions now have a life expectancy of their own.
“Malaria is a very smart disease,” Filler said. “Both the mosquitos and the parasite itself really can thwart biologically what we try to do.”
The challenge then becomes keeping the pipeline packed with new drugs. It’s what Magill and other experts call “feeding the beast.” Pharmaceutical company Novartis has two new drugs in development that will attack the two most virulent forms of the disease. While both are promising — KAF156 is the first drug with strong potential to kill the P. vivax and P. falciparum malaria parasites at an early, asymptomatic stage — neither are single-dose treatments.
Single-dose treatments are favored by doctors because they reduce the chance that a patient won’t finish their treatment regimen or that they will give away remaining pills to family members. Patients who stop treatment prematurely aren’t cured, even though they might feel better. What’s worse, when patients stop treatment too early, a parasite is more likely to develop resistance.
See more related stories:
● The future of the fight against malaria
● Innovations for malaria control: Advancing progress for a healthier, more prosperous world
● Solve for M: 5 key challenges to ending malaria
● Target 'zero': Going full force against malaria in Asia
Currently, as few as just one viable single-dose treatment appears to be in the human trial phase, according to the Fogarty Center at the National Institutes of Health: a single-dose treatment created by the British pharmaceutical giant GlaxoSmithKline called tafenoquine, developed in partnership with the Medicines for Malaria Venture.
GSK also has a vaccine in the works, called RTS,S, which is also in clinical trials in partnership with the PATH Malaria Vaccine Initiative. RTS,S is meant to protect young children and infants in malaria-endemic parts of the world. Questions remain about its effectiveness; an early trial suggested only 50 percent protection against the parasite.
But is RTS,S a silver bullet? Not quite, says to Todd Summers, senior adviser to the Center for Strategic and International Studies’ Global Health Policy Center in Washington, D.C.
“It’s one more tool that you use at the right place at the right time,” he told Devex.
This is relatively new territory. The word vaccine easily conjures images of an all-encompassing cure. The smallpox vaccine — which eliminated the disease — is the poster child of silver-bullet interventions and may set a dangerous expectation for today’s more complex disease initiatives. Farmers were “vaccinating” themselves against smallpox using cowpox for hundreds of years before the World Health Organization undertook its eradication campaign in 1967. After that, it took only 14 years to banish the biblical disease from the planet.
Without a single-dose treatment for malaria, keeping the public and donors encouraged year after year, budget season after budget season, requires a shift in global health perspective, one that embraces the ever-changing spectrum of anti-malaria tools.
For Summers, potential and current donors must get comfortable taking on malaria without a silver bullet. Indeed, what’s proven most effective in the last two decades has been the combined use of several tools: treatment with malaria medicines, diagnosis tools like rapid diagnostic tests, reduced transmission through bed nets, insecticides and indoor residual spraying, and the continued development of vaccines.
“The deployment of all four at significant scale — even if it’s different formats for different countries — has made a huge impact,” Summers said. “The package is the silver bullet.”
The road ahead
A man walks down a rural road in Mali, his donkey so loaded with brightly packaged medical supplies, drugs, bed nets and other interventions that the two look like a traveling circus. To Summers, this image, taken a few years ago, illustrates the challenge of, well, addressing complex health challenges.
And malaria isn’t the only disease which requires a multifaceted response. When three, four or five tools are needed to treat just one disease in a rural community that’s facing multiple health challenges, logistics can get hectic. Making matters worse, many diseases overlap. Co-infection of tuberculosis and HIV in Ukraine, for example, is high.
Pneumonia and malaria share treatments, for instance, as do pneumonia and diarrhea.
But for the longest time, global health financing was largely disease-specific. The Global Fund, for instance, focuses on malaria but not pneumonia, even though the diseases are often confused in early stages and could theoretically be treated simultaneously.
In order to get more bang for a donor’s buck, Magill said, pairing disease efforts is the obvious answer.
“The system is pointing toward a more integrated delivery model,” he said.
“And politically,” Summers added, “that makes things a little more salable. Because then you’re saying [to donors], we can be even more efficient by combining our interventions.”
Double disease initiatives are becoming more common. Tuberculosis and HIV campaigns have proven effective in Ukraine and Russia, for example, where co-infection is on the rise.
Advocates agree that funding cuts, even for a short period, could be devastating. A majority of the 75 malaria resurgences since 1930 can be attributed to funding cuts, according to a study by the Clinton Health Access Initiative.
“We know if you stop investing in malaria control, it comes roaring back,” said Martin Edlund, founding member and CEO of Malaria No More.
“And those who have been infected lose immunity, and are more at risk than before.”
What has often been called the greatest boon for anti-malaria advocates — that results are quick and the benefits of funding are easily measured — is also the greatest weakness. Any stall in funding means the disease will quickly rebound, potentially stronger than before.
“Even missing the distribution of bed nets for just one rainy season,” Summers said, “and you see child mortality rise about as quickly as the statistics can be gathered.”
And every missed opportunity to end the disease means more interventions will likely be lost to drug-resistance. It’s what happened after the use of DDT was banned beginning in the late 1960s. It’s a destructive pattern: waves of funding nearly eradicate the disease, then complacency sets in and disease resistance and resurgence occur.
New sources of funding
While there are concerns the new, Republican-led U.S. Congress will mute its support for malaria eradication, other donors are stepping up. The Bill & Melinda Gates Foundation has become one of the nonprofit supporters of anti-malaria initiatives, contributing $192 million to R&D and control initiatives in 2013, according to the Kaiser Family foundation.
Oil and gas companies, in particular, have begun to support anti-malaria initiatives as their staff and the communities in which they work are particularly threatened by the parasite. Chevron, the Global Fund’s largest single corporate partner, is providing $60 million over eight years to the financial institution. The ExxonMobil Malaria Initiative supports prevention, control and treatment programs in Nigeria, Chad, Cameroon, Equatorial Guinea and Angola.
The private sector can play a huge role in the fight against malaria, experts agree.
“I think the big area where there needs to be more attention is the indigenous private sector,” Pender said. “We’ve struggled to really harness that potential.”
Private sector investments in anti-malaria efforts would have to increase significantly if government funding drops next year. So fundraisers are looking to elsewhere, to investment banks and other domestic, regional and global players.
International financial institutions like the World Bank could serve as brokers — they work closely with finance ministers, who tend to have more leverage over national budgets than the health officials who work closely with the Global Fund. The Asian Development Bank, for example, launched the Regional Strategic Response to Malaria and Other Infectious Diseases initiative in late 2013, followed closely by a slew of country-based campaigns last year.
The proliferation of country-level malaria initiatives is crucial, not just because of potential funding cuts next year. As global wealth grows, even the poorest countries in Southeast Asia and sub-Saharan Africa, where malaria burdens are high, will graduate to higher-income brackets in the World Bank’s income classification system. That’ll prompt the loss of critical support: Governments will no longer be eligible for concessionary pricing on medicine, insecticides and bed nets, among other things — a perfect moment for malaria to bounce back yet again.
“Great graduation present, right?” Summers quipped.
Institutions using the bank’s income classification system, like the Global Fund and Gavi, the Vaccine Alliance, are taking a hard look at how they draw that line and whether they’re doing everything they can to prepare countries for graduation.
“Domestic financing doesn’t keep up, and there’s very little evidence that the Global Fund is inviting or enticing countries to put more money on the table so that it can get out,” Summers said.
The Global Fund’s senior disease coordinator for malaria disagrees. The fund asks governments that seek malaria funding to provide detailed plans and cost estimates — a powerful leverage, Filler suggested.
“We can say, ‘Your country needs 12 million bed nets and we’re going to finance 10. You need to finance two more,’” he said.
Asked about the future of the anti-malaria movement, Filler highlighted the importance of emerging economies of India, Brazil and China to become Global Fund donors. Regional cooperation — neighbor helping neighbor — could become more common, he said, as countries move closer to eradication.
Just as epidemiologists have learned to stop searching for a silver bullet and instead concentrate on filling the malaria drug pipeline, many anti-malaria advocates see the looming funding crisis as a cue to maintain a constant flow of funding by tapping alternative sources of support.
What’s the biggest threat we’re facing today in the fight against malaria? Let us know by leaving a comment below.
Riley Brands contributed reporting.
Join the Devex community and access more in-depth analysis, breaking news and business advice — and a host of other services — on international development, humanitarian aid and global health.