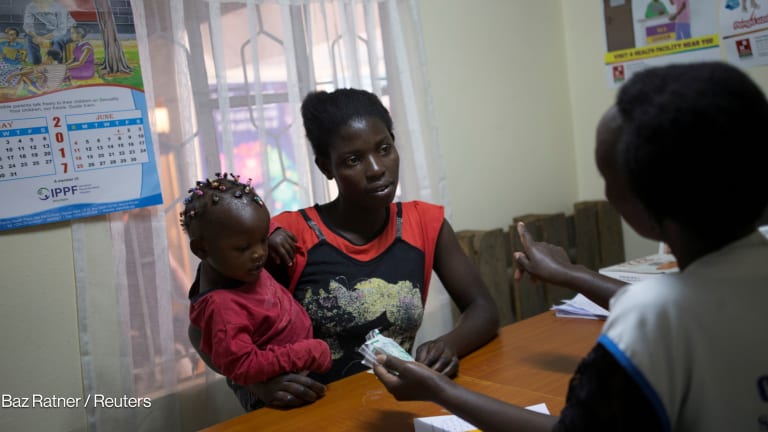Two years in, report finds 'global gag rule' cuts access to health care

NEW YORK — More than two years after the Trump administration’s implementation of the expanded “global gag rule,” the impacts of the U.S. policy are increasingly clear: the regulations are cutting access to all health services, according to a new report from the International Women’s Health Coalition.
The Mexico City Policy — which states that foreign NGOs that receive any U.S. global health funding are prohibited from engaging in abortion-related activities, including providing counseling or education — had an instant chilling effect on those organizations, forced to choose between providing abortion-related services and receiving U.S. global health funding.
“We are seeing the disintegration of health services.”
— Jedidah Maina, executive director, Trust for Indigenous Culture and HealthBut the full impacts for NGOs and other health providers have unfolded with time, as well as the extent the new policy is forcing organizations — and even governments — to recalibrate the way their do their work.
Global gage rule news:
► In Nigeria, Trump administration policies bite hard
► US gets a C on sexual and reproductive global health assistance, new index finds
► Forced to choose between US and Swedish funding, sexual health NGOs speak out
“This policy is really hurting people’s health, in particular women’s and girls’ health and the health of the most marginalized populations. It is affecting not only sexual and reproductive health services and abortion services, but it is also affecting nutrition, maternal health services, gender-based violence and all different types of things,” said Vanessa Rios, an IWHC program officer at a media briefing in New York.
“The impacts of the policy are very widespread and it is literally killing women,” added Rios, the author of the “Crisis in Care” report released June 5 at the Women Deliver conference in Vancouver.
The report, based on more than 170 interviews with civil society organizations, health service providers, and government agencies in Kenya, Nepal, Nigeria, and South Africa, outlines some of the policy’s impacts.
Two women died following self-induced abortions in Kenya after a local sex worker organization signed the policy and stopped providing abortion services and referrals, according to the report. In Nepal, an organization implementing a USAID family planning project did not accept the conditions of the rule and ended its work early, stopping outreach work in 11 rural districts. Other organizations said they are afraid to participate in training sessions or conferences that might address abortion, the report said.
The organizations face a difficult choice in choosing to accept the policy or not, and both decisions have impacts, said Françoise Girard, executive director of IWHC. “Either way, you are left in a lurch,” he said.
The report also revealed an unexpected impact on governments — even those with liberal abortion laws. While governments themselves are exempt from the policy, they now cannot contract out work to some civil society organizations that previously provided a bulk of the country’s health services, because they signed on to the MCP.
“It affects the work of governments pretty significantly. That was something we did not expect to see, to that extent,” Girard said.
The policy has a wide reach — the U.S. is the largest global health donor and its $10.8 billion in fiscal year 2018 funding was nearly quadruple the amount of the U.K., the second largest donor. At least 1,275 foreign NGOs have likely been impacted by the policy, the Kaiser Family Foundation reported in December 2017.
Because policy applies to new contracts, some organizations have only begun to see the full extent of the agreement’s effects over the past several months.
In some cases, health clinics in remote areas can no longer provide comprehensive health care. And people from marginalized communities are much less likely to seek specialized care if it is not available at a local health clinic people may rely on, according to Jedidah Maina, executive director of the Nairobi-based grassroots organization Trust for Indigenous Culture and Health.
“We are seeing the disintegration of health services. In the run-up to the global gag rule, there was more of a one-stop-shop for all reproductive health services,” Maina said at the briefing. “If that facility is providing more comprehensive services people are more likely to go there. If they are given one type of treatment and told to come back tomorrow, most likely that is an opportunity cost they do not want to take.”
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5