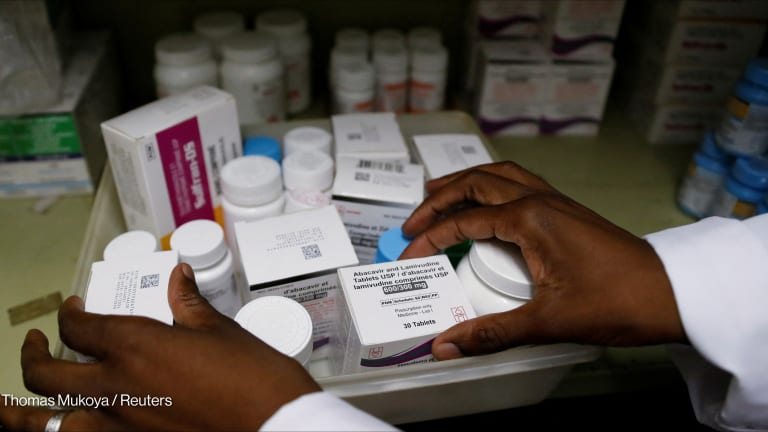
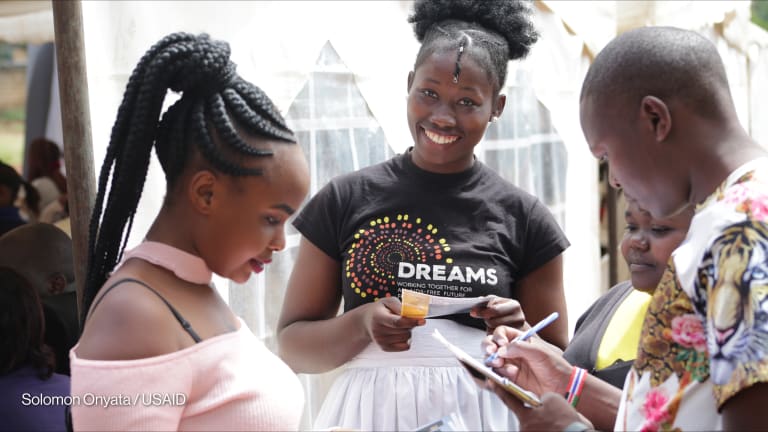Uncertainty over PEPFAR support prompts concerns from HIV advocates in Nigeria

LAGOS and RIVERS STATE, Nigeria — Dr. Bola Oyeledun arrived at General Hospital in Kafanchan, Kaduna State in 2005, during the peak of Africa’s HIV and AIDS epidemic. Scores of patients awaited her. An emaciated, possibly HIV-positive baby was rushed to her attention by a distressed head nurse and the mother who, sobbing, begged Oyeledun to save her child. She couldn’t.
Oyeledun had traveled to Nigeria at the behest of ICAP, at Columbia University, which had kicked off operations in the country that year with funding from the U.S. President’s Emergency Plan for AIDS Relief. The center’s mandate in Nigeria was to deliver initiatives providing quality care while ultimately transitioning responsibility to local organizations.
Largely thanks to PEPFAR’s support, the situation has changed dramatically over the last 13 years. Across Nigeria’s 33,000 health facilities — 4,000 of which provide HIV and AIDS care — it is rare to find a hospital ward filled with patients with AIDS. HIV prevention messaging is no longer the taboo topic that it once was.
As of June 2017, PEPFAR had invested more than $5 billion in Nigeria. That funding has provided antiretroviral treatment for 880,668 people, HIV testing for 7.76 million people, and care and support for 1.28 million orphans, vulnerable children, and their caregivers. The number of yearly new infections has edged downward from an estimated 316,733 in 2003 to 239,155 in 2013.
Nigeria accounts for 9 percent of the global HIV burden.
—“We have made tremendous progress,” Oyeledun told Devex. But Nigeria’s HIV epidemic is still far from controlled.
With more than 3.4 million people living with the virus, Nigeria accounts for 9 percent of the global HIV burden. The population stands at 190 million and is growing quickly. Half of Nigerians are under 30 — the median age is only 18 — exactly the age bracket most at risk of being infected with HIV.
Such demographics — which are also present in many other AIDS-affected African countries — continue to justify the word “emergency” in PEPFAR’s acronym, as Mark Dybul, former executive director and one of the initiative’s key architects recently argued. In late April, he said these trends — along with insufficient global funding — mean, “we are … at highest risk ever of losing control of the epidemic since all of this began.”
Nigeria is key to maintaining control of Africa’s epidemic. But total PEPFAR funding for the country, including both new funds and those in the applied pipeline, has dipped, falling from $409.1 million in 2016 to $383.6 million for 2017. The budget numbers for 2018 have not yet been released.
Meanwhile, President Donald Trump’s administration has proposed cutting about 18 percent of PEPFAR’s global budget. While that proposal has so far been flatly rejected by U.S. Congress, it has compelled PEPFAR and its partners to scrutinize their spending.
Against this backdrop, in September 2017, PEPFAR unveiled a new strategy, which identified 13 focus countries where it will accelerate efforts to achieve epidemic control. Nigeria was not among them.
The country was left off the list in part as a “wake-up call” for its government and those engaged in addressing the epidemic in the country — a bid to make them question and examine why they were left out, said U.S. Global AIDS Coordinator Deborah Birx, who leads PEPFAR.
In addition, Nigeria wasn’t made a focus country, largely because PEPFAR doesn’t understand the breadth and depth of the epidemic, making it difficult to respond equitably, she said.
“You can't plan a program and what the resource needed are, when you really don't know how many HIV positive clients there are.”
—Deborah Birx, U.S. Global AIDS CoordinatorTo better understand the challenges, PEPFAR, along with the Nigerian government, is conducting a $125 million survey to define the epidemiology of HIV in the country, Birx told Devex.
“We're 30 years into the pandemic and we're going to finally know what the prevalence is with a confidence interval of 0.5,” Birx said. “You can't plan a program and what the resource needed are, when you really don't know how many HIV positive clients there are — how many women, and children, and men.”
Even with PEPFAR’s support, health services have never been adequate, experts said. And despite this, the Nigerian government has decreased the percentage of its budget dedicated to health over the past decade and recently lost funding from the Global Fund to Fight AIDS, Tuberculosis and Malaria as a result of not meeting its financial commitments.
PEPFAR implementers in some high-burden states fear that if they leave — even as part of a previously planned transition — the state governments won’t be able to step up to the plate.
And with Nigeria’s youth boom, much is at stake.
The need for government buy-in
While UNAIDS targets call for 90 percent of people with HIV to know their status, only 34 percent of Nigerians do.
—While Nigeria has made enormous strides in addressing the epidemic — 88 percent of people who know they are HIV-positive are on treatment, and 81 percent of them have achieved viral suppression — advocates point to many remaining challenges.
Across the country, there aren’t enough facilities providing HIV services, and the quality of care is often inadequate, according to Ibrahim Tajudeen Olaitan, acting executive secretary of the country coordinating mechanism for the Global Fund in Nigeria. While UNAIDS targets call for 90 percent of people with HIV to know their status, only 34 percent of Nigerians do.
Compounding concerns over PEPFAR funding is the fact that while the initiative was designed to work in tandem with the government, many HIV leaders and implementers say Abuja’s commitment has been insufficient.
PEPFAR’s most recent figures show that it funds 64 percent of HIV investments in Nigeria, while the government provides 27 percent of the funding.
“[Nationally], health is seen as a charitable thing in Nigeria and not an investment,” said Emmanuel Funsho-Adebayo, lead consultant for the nonprofit Health Strategy and Delivery Foundation.
“This government has had the lowest budget dedicated to health [compared to previous administrations] in the last 10 years,” said Funsho-Adebayo.
The 2018 budget, passed in June, allocated 3.9 percent to the health sector, according to an analysis by BudgIT, a Nigerian pro-transparency NGO. Government data shows that the highest allocation in the past decade was 5.95 percent in 2012.
This is despite the fact that in 2001, Nigeria committed to spending 15 percent of its budget on health in the “Abuja declaration.”
The spokesperson of the Federal Ministry of Budget and National Planning, James Akpandem, said that a larger national budget overall means the health budget has actually increased 33 percent. He added that there is also money spent on power, works, housing, and water — which supports health infrastructure but comes out of a separate budget.
The Federal Ministry of Health did not respond to repeated requests for comment.
The Health Strategy and Delivery Foundation works in seven high-HIV-burden states, connecting state governments and PEPFAR implementing partners, and complementing their work. The organization, which is currently working on a project to curb mother-to-child transmission, provides its data to PEPFAR implementing partners who use it to execute their work in partnership with government. While the project is expected to end in September, having prepared health systems to operate on their own, Funsho-Adebayo fears that when HSDF leaves, the systems in place might not be properly supported.
“When we leave, even though we have prepared the government they still need funds to implement,” Funsho-Adebayo told Devex, explaining that the state government doesn’t allocate sufficient financing to meet the health sector’s needs.
Olaitan said he believes PEPFAR’s new strategy is aimed at pressuring the Nigerian government to deal with its inefficiencies.
“Looking at the population at risk and the current coverage, we need to still continue expanding services. The Nigerian government needs to fill the gap,” he said.
“Looking at the population at risk and the current coverage, we need to still continue expanding services. The Nigerian government needs to fill the gap.”
— Ibrahim Olaitan, acting executive secretary of the country coordinating mechanism for the Global Fund in NigeriaThe Global Fund’s role is basically that of a gap filler, “supporting programs run by local experts and countries most in need.” But Olaitan stressed that the Global Fund will not be filling any holes resulting from any funding cuts or change in strategy by PEPFAR.
In fact, Olaitan said that the Global Fund has pulled some funding from Nigeria because the government had not fulfilled counterpart funding commitments. He revealed that in 2017, Nigeria lost 15 percent of earmarked funds — about $170 million — originally allocated by the Global Fund. The money was decommitted because the government could not provide evidence that it had matched 15 percent of the fund’s health spending in Nigeria between 2014-2016.
Now, the government needs to fulfill the Global Fund’s preconditions before it receives more funding. This means providing a letter of commitment clearly stating where the money will be sourced from. If it once again can’t be accounted for, the country stands to lose 15 percent of the funding for the 2017-2019 period, according to Olaitan.
For his part, Walter Ugwuocha, executive secretary of the Civil Society for HIV/AIDS in Nigeria — a coalition of groups working on HIV and AIDS — took a hard line on engaging with the Nigerian government on combating the virus.
“If you want them to act, pull out completely,” he said.
Concerns among local implementers
In Benue, a high-HIV-burden state implementing PEPFAR, the Centre for Integrated Health Programs — the product of Oyeledun’s work with the International Center for AIDS Care and Treatment — debuted a treatment scheme in November 2015 in Nigeria. It took HIV testing to the doorsteps of hard-to-reach communities.
“When we compared data over time, within the first year of implementation, we got over 40 percent of the people testing positive — people who otherwise would not have gone to a health facility to be tested,” Oyeledun said.
The organization would then look to start them on treatment immediately, linking them to the closest primary health care centers. But CIHP would later find that those primary health care centers were dealing with their own laundry list of challenges.
Often, health centers in rural areas were not adequately staffed to offer first-rate HIV testing or counseling services, and as such, were easily overwhelmed — a problem that persists today. Many clinics did not have adequately trained data personnel, leading to information on infected persons to be entered incorrectly, incompletely, or not at all. In addition, the centers often did not have resources to work efficiently with reliable electricity in constantly short supply.
CIHP initially decided to do the work itself to make up for these gaps, supplying health centers with technical personnel to provide counseling services and record data. But facing funding cuts, CIHP changed tack, looking to train and build the capacity of the health centers.
In 2017, PEPFAR funding for the program ended, shuttering their operations. Oyeledun said the program had been making significant headway and that while PEPFAR would continue to provide antiretroviral medicine and other services through a new partner, she felt that they were abandoning the community.
“We had built trust, capacity in the community, and yet we were told to leave. It is not good for continuity,” Oyeledun said.
Dennis Otobo has seen firsthand what can happen when this transition isn’t handled properly. Working in Rivers State, Otobo is the director of Status for Youth Development and Total Health Initiative, a grassroots organization which previously received funding from PEPFAR through its implementing partner, FHI 360.
“We had built trust, capacity in the community, and yet we were told to leave. It is not good for continuity.”
— Dr. Bola Oyeledun, chief executive officer at CIHPOtobo explained that when partners stop supporting a particular health facility — for instance drawing back on resources or capacity building — staff in such facilities often do not continue the efforts. Where the partner had provided knowledge, such as counseling techniques and maintenance of testing equipment, these needs may not be followed through at the same standard.
“There is no ownership or sustainability measures put in place,” he said.
PEPFAR should divert some of its funding to advocating and sensitizing the political class about the importance of sustainability structures, Otobo added.
Golden Owhonda, director of public health and disease control at the Rivers State Ministry of Health, said these issues are being addressed.
“A lot of hospital personnel have been trained on service delivery. In terms of manpower, we don't have a shortage, but we could have shortages in terms of commodities, equipment because of [a lack of] recurrent funding for it. Those could have shortfalls,” he told Devex.
An uncertain path forward
Owhonda told Devex that Rivers State is preparing for shortfalls in PEPFAR funding.
It is currently in the process of setting up a “domestic resource mobilization committee,” which would explore funding from alternative sources, particularly the private sector — including oil and gas multinationals operating in the state. This is an all-hands-on-deck process with the government, community-based organizations, NGOs, and civil society groups involved, Owhonda said.
15 years later, PEPFAR is still at war with a global epidemic
On May 27, 2003, U.S. Congress authorized the largest-ever investment in a single disease in U.S. global health history. Fifteen years later, PEPFAR has saved millions of lives and transformed global development.
The effort is being spearheaded by the Health Finance and Governance Project, created and funded by the U.S. Agency for International Development, which seeks to ensure countries’ “health gains are preserved.”
But the initiative has not had much success over the past 1 1/2 year of operation, according to Owhonda and Otobo.
There is now an impasse between government and civil society groups about how the alternative funding body should be run, with civil society groups concerned that if the government controls the funds, there will be little accountability and they might be diverted, Otobo said.
In addition to those tensions, the committee is finding it hard to raise money to begin with, Owhonda said.
“There's a lot of government desire. We’ve made quite a number of efforts to get private sector to support HIV treatment, but it hasn't yielded the desired result,” he said. “It is either too early to judge, or we could say we are short of targets.”’
The state is also exploring another solution, already piloted in other states across the country: VIP clinics. It will be user fee-based, marketed to the well-heeled seeking HIV treatment, offering perks, such as increased privacy and refreshments while awaiting doctors. Owhonda explained that the money made from those clinics would then be directed toward public hospitals, providing care for those who might not be able to afford it otherwise.
Also in the works is universal health insurance, with a bill currently being debated in the Rivers State legislature, Owhonda said.
This is also a priority at the national level, with the 2018 national budget setting aside 1 percent of its projected revenue toward UHC. Discussions are underway with the National Health Insurance Scheme to include HIV services under this coverage. This intervention is separate from the 356 billion naira ($990 million) expenditure allocated to the Federal Ministry of Health. Additionally, the National Assembly allocated 55.15 billion naira in enforcement of a National Health Act passed in 2014, but largely ignored until now.
Speaking at Devex World about the fight against the virus in sub-Saharan Africa more broadly, Dybul said that one of the major problems advocates face now is that traditional HIV programs don’t necessarily reach today’s youth.
PEPFAR has commissioned one of the largest HIV and AIDS indicator surveys in the world in Nigeria.
—“Survey[s] show that they don’t even care about HIV anymore; they don’t think about HIV. They think about jobs, reproductive health, their community, their friends, their family. They think about what everyone else thinks about,” he said.
The future of PEPFAR in Nigeria may be clearer in the next year if it solves one of its biggest challenges: Accurate data. PEPFAR has commissioned one of the largest HIV and AIDS indicator surveys in the world in Nigeria, set to kick off in June 2018 with preliminary estimates expected in the last quarter of the year.
According to Olaitan, the survey will answer a number of questions on the response to the epidemic. These include whether interventions are reaching the right people, how rural and urban areas are impacted differently, current coverage levels, and what types of services health facilities are providing.
Dybul called for advocates to look to local communities for solutions, and view at-risk youth as “person with potential” to be supported in healthy, productive lives.
“That will get us way past health, way past individual diseases, and instead focused on what we need for human beings for their future and their potential.”
Adva Saldinger and Michael Igoe contributed reporting to this article.
Update, July 18, 2018: This article has been updated to clarify that Dr. Bola Oyeledun had traveled to Nigeria at the behest of ICAP, at Columbia University.
Update, August 3, 2018: This article has been updated to clarify that Oyeledun worked at General Hospital in Kafanchan, and that the baby rushed to her may have been HIV-positive but that it was not confirmed. The number of patients on a waitlist for treatment — 6,000 — has been removed as the patients were registered at a different hospital. It has also been updated to reflect that CIHP’s work in Benue was handed over to a new PEPFAR-funded partner.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5