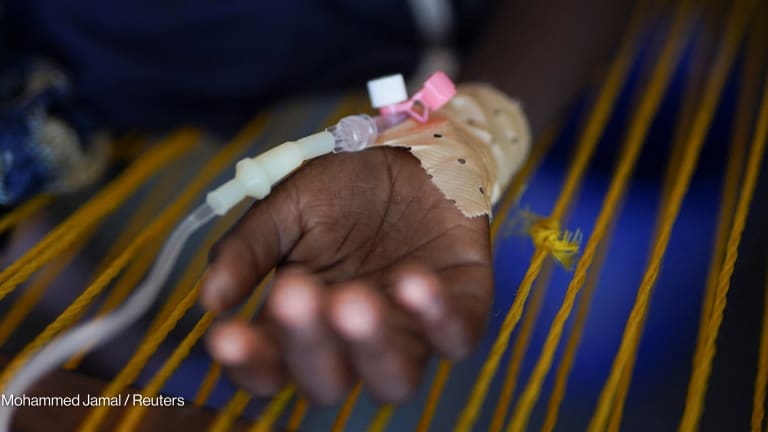
Burao, SOMALILAND — On a recent afternoon, six patients remained in a cluster of tents making up the cholera treatment unit in the Togdheer region in central Somaliland. Most of the other beds were empty and the last patients were on the path to discharge. A recovering 1-year old boy named Abdirahman scurried through the children’s inpatient tent giggling.
Dr. Abdillahi Ali Musa remembered more somber days. When the outbreak peaked in June, he and other doctors here were treating over 200 new patients in a day, 70 more than their entire bed capacity. Two twins Abdirahman’s age were admitted too late to be saved, among the nearly 300 deaths recorded by the Somali Red Crescent Society during the outbreak. The SRCS treated over 12,000 cases in the Togdheer region alone, 70 percent of the total cases in Somaliland.
Cholera infections spread through contaminated food or water. In recent years as more severe, drug-resistant strains of the bacteria have emerged, both the frequency and length of global outbreaks have increased. Amid a civil war and collapsing public service system, Yemen saw the largest cholera outbreak in recent history this year, with over 860,000 suspected cases and over 2,000 deaths.
In Somaliland, cholera is a symptom of drought. Rainy seasons in the Horn of Africa have disappointed for three consecutive years, now heading into the fourth. As crops fail, livestock die and boreholes dry up, communities drink whatever water they can find. Prolonged malnourishment compromises immune systems, making patients more susceptible to cholera. According to Oxfam, cholera has been associated with more than 1,500 deaths this year in this part of Africa.
Cholera is also a symptom of weak health and water systems, and ultimately, lack of access to universal health coverage, said Amanda McClelland, health security and risk management advisor for the IFRC. “These outbreaks tend to occur in areas where surveillance systems pick up the outbreak much later,” she said.
The disease is endemic in Somaliland, but for the moment, the country has curbed its outbreak. The humanitarian strategy, led by the Somali Red Crescent Society, included deploying community-based volunteers, increasing public health education, and coordinating with the government. Relief efforts are now working with Somaliland’s Ministry of Health to prevent another outbreak and ensure that if and when cholera returns, the government can take greater ownership of the response.
Somaliland’s unique experience is particularly important as the global public health community aims to curb deaths from cholera. In October, the Global Task Force on Cholera Control, a network of U.N. and international agencies, academic institutions, and NGOs, launched a strategy to globally reduce deaths from cholera by 90 percent by 2030. The strategy aims to better coordinate efforts by governments, donors, and technical partners, as well as to strengthen water, sanitation, and hygiene efforts in hotspots and improve early detection.
“Nobody should die from cholera,” said Dorothy Francis, acute watery diarrhea, drought and food security operations manager for International Federation of Red Cross and Red Crescent Societies Somalia Country Office. “People die from cholera when they don’t know what’s happening, and when they don’t get help quickly.”
The outbreak
Cases of cholera began to pop up in Somaliland in late 2016, following the failure of two rainy seasons. Health workers say it became difficult to convince people to use limited stocks of water for sanitation. Without toilets in many rural areas, open defecation can seep into groundwater. The disease spread further as nomadic populations moved from place to place in search of water, including across borders. Internally displaced persons camps also became hotbeds of cholera, because of the absence of latrines and clean water. Cases continued to rise throughout the spring.
Somaliland unilaterally declared independence from Somalia in 1991, but this independence has not been recognized by the international community. Since then, Somaliland has been independently governed, with its own decentralized ministries. The national government places high priority on security spending, leaving only 4 percent of its budget for health, said Ahmed Bakal, Somaliland coordinator for the SRCS. With this limited budget, the Ministry of Health prioritizes hospitals in urban areas.
Mobile clinics bring stable care to moving populations in Somaliland
Nomadic communities are among the most challenging populations to reach with consistent health care. The International Federation of Red Cross and Red Crescent Societies is using a system of mobile clinics in Somaliland to reach these roving populations. Devex goes inside the operation to understand how it works and what lessons it might hold for reaching patients on the move.
The SRCS and other organizations work to fill the gaps in rural areas. The SRCS has 33 fixed clinics and 33 mobile clinics in Somaliland funded through the International Red Cross community, in collaboration with UNICEF and other U.N. agencies. Services are free of charge, said Bakal.
The SRCS clinics are equipped to handle acute watery diarrhea, but a large cholera outbreak could quickly overwhelm the system.
In April 2017, as the crisis grew, the national society decided to scale up its response, applying for funds from the IFRC’s revolving Disaster Relief Emergency Fund, a global facility that provides rapid emergency financing.
In May, the IFRC and SRCS conducted a rapid assessment in some of the worst-affected areas and realized that the outbreak was worse than initially believed. In response, IFRC deployed an emergency response unit in May, supported by the Canadian Red Cross and the Norwegian Red Cross. Emergency responders established a cholera treatment center in Burao — a group of tents that included inpatient and observation wards. A few smaller cholera treatment units were also deployed in hotspot areas.
SRCS also launched an education campaign in Burao. They distributed 20,000 flyers and drove through villages and towns broadcasting messages on cholera prevention from loudspeakers on top of vehicles. They urged residents to chlorinate water, build latrines, and avoid open defecation. Public places such as markets and schools broadcasted a documentary film on cholera prevention. Faith leaders were also looped into the efforts. During Friday prayers, these leaders would teach community members about hygiene and sanitation practices, such as hand washing.

Health volunteers
IFRC trained and deployed unskilled health workers as Somali Red Crescent Society volunteers to run 43 oral rehydration points in outbreak hotspots. The volunteers became the first point of contact for patients coming in for cholera or acute watery diarrhea and were trained how to physically examine a person, for example, by pulling their skin to check the patient’s level of dehydration.
Volunteers gathered basic information from the patient, such as the frequency of their stool, and categorized patients by severity. Acute cases were referred to the cholera treatment centers and units where trained health professionals could prescribe antibiotics and IV treatments. For mild and moderate cases, volunteers offered oral rehydration salts, zinc, and soap, and then sent patients home.
After each day of work at an oral rehydration point, volunteers sent a text message to a data manager in the capital city of Hargeisa, reporting the number of cases they handled, including patient details. The idea for an SMS reporting mechanism emerged after the 2012 outbreak of cholera in Sierra Leone, said McClelland of IFRC. The constant data stream in Somaliland helped the IFRC pivot its response based on needs, whereas before the organization would wait until the end of the crisis to sift through paper records.
Volunteers were crucial to lessening the load on skilled medical workers. Ninety percent of cases were handled in the oral rehydration points, said Kaltuun Hussein, national health officer for SRCS. The teams were also mobile, offering a cost-effective, community-based response. Local volunteers were also vital because expat relief workers are unable to travel to many parts of the country because of security concerns, said McClelland.
“The unique part of the Somaliland response is the difficult security context,” she said. “We made sure we got care out to the lowest level, even when we couldn’t necessarily get there in terms of medical support teams.”
Volunteers also helped demystify the treatment of cholera, said Kwame Darko, health delegate to the IFRC Somalia Country Office. The disease can now be viewed as something that can be tackled by communities, not only in clinics and hospitals. Volunteers are part of IFRC’s strategy to reach last mile populations with universal health coverage, by expanding the network of health providers.
Government participation
Somaliland’s Ministry of Health does not have an early warning system in place to spot a cholera outbreak, said Hussein. Hospitals and clinics collect their own data, largely without sharing.
Even if the government had been alerted early, social stigma is an enormous barrier to combatting cholera. The government has been hesitant to use the word “cholera,” preferring the term “acute watery diarrhea,” said Hassan Abdi Jama, deputy national health officer for SRCS. Acute watery diarrhea is a symptom of cholera. In severe cases, if left untreated, cholera can kill within a few hours. If it’s not contained, the disease can spread across borders, making many governments fear that being transparent about a cholera outbreak could negatively hit sectors such as tourism and trade.
Despite the disincentives, however, the Somaliland government worked to ensure the cholera response teams were able to move quickly, said Bakal of the SRCS.
At the onset of the outbreak, Somaliland President Ahmed Mohamed Mohamoud gave an order to all government agencies to support the Red Cross in its outbreak response. When equipment arrived in the Port of Berbera, on Somaliland’s coast, it was instantly released, even without the usual customs paperwork, said Bakal. Tax-exemption paperwork usually must be processed through the Ministry of Health, Ministry of Planning, and Ministry of Finance, as well as payment of port charges, before equipment is released, he said. This can take at least a week.
Throughout the outbreak, the IFRC worked to increase the capacity of the government. The cholera treatment center in Burao was staffed by a mixture of Ministry of Health workers, as well as the SRCS, who were training the government workers throughout the crisis, said Francis of IFRC.
Daily coordination meetings between U.N. agencies, local NGOs, and the government also improved capacity, said Jama.
IFRC emergency response units are intended to provide a country with relief for up to three months. So as the outbreak wound down, the cholera treatment center was broken down into smaller cholera treatment units. The equipment has been handed over to the government’s Ministry of Health. A warehouse is being built in Burao to store the treatment units, which will be at the government’s disposal for deployment during the next outbreak. The IFRC will also hold a training in November for the Ministry of Health.
“This has been an eye-opener to try to put things on the right track for future emergencies,” said Darko. “It was a wake-up call.”
The next outbreak
Somaliland’s cholera outbreak was successful because of the coordinated international response, willingness of the government to allow responders to operate without restrictions, and the use of volunteers at the oral rehydration points to not only reach areas that were difficult to access because of security concerns, but also lessen the load of the trained health workers.
Somaliland is not in the clear yet. The Deyr rainy season is expected to have below-average rainfall in the Horn of Africa, according to the Famine Early Warning Systems Network. This is expected to exacerbate a situation that has already left an estimated 15 million people facing food insecurity. Somaliland will likely face emergency food insecurity until at least January, according to Oxfam. Another outbreak could hit the country again as the water crisis continues to cripple the region, weakening immune systems and pushing people to drink contaminated water.
Cholera can enter countries in times of crisis, as happened in Somaliland, but outbreaks are also exacerbated by already weak health systems. The weak health infrastructure in Somaliland and delay by the government to acknowledge the outbreak contributed to the ability of the outbreak to reach the levels it did, said Francis. In the future, the SRCS is hoping the government will take more ownership over outbreaks of cholera, including implementing early detection systems.
The IFRC is currently paying for the Ministry of Health staff salaries in the cholera treatment unit that remains in Burao. Starting December, the government will be responsible for paying the salaries. It’s unclear whether the funding will be there, said Darko.
Despite efforts to build the government’s capacity, the process is slow moving, said Francis. The SRCS expects to continue to play a support role to the government when the next cholera outbreak hits Somaliland.
Editor’s note: IFRC facilitated Devex's travel and logistics for this reporting. However, Devex maintains full editorial control of the content.
How do we ensure that people worldwide get the care they need without the risk of being pushed further into poverty? Devex explores the path to universal health coverage. Join us as we ask what it will take to achieve UHC for all by visiting our Healthy Horizons site and tagging #HealthyHorizons, #Health4All and @Devex.
The content, information, opinions, and viewpoints in this Healthy Horizons content series are those of the authors or contributors of such materials. Content produced as part of the series does not represent an endorsement of the contributing institutions or their positions, nor does it imply the existence of any relationship or engagement among them in connection with this series.