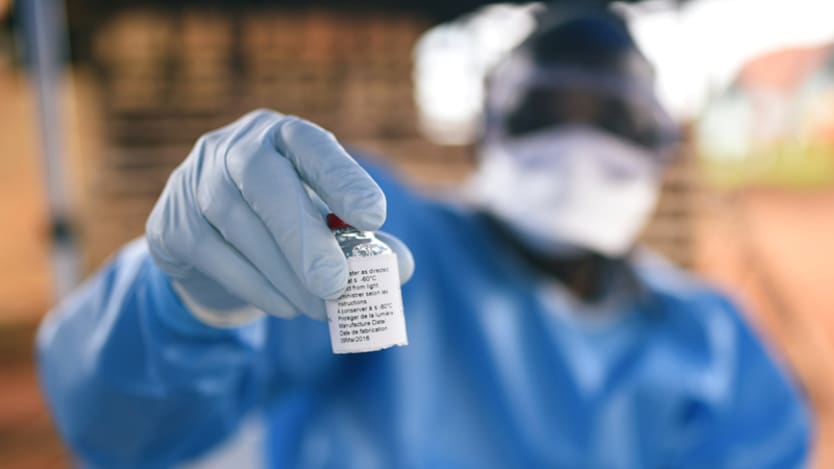
NEW DELHI — The Democratic Republic of the Congo is currently facing the most severe Ebola outbreak in its history, with over 400 deaths confirmed since August, according to the World Health Organization. Much hope is pinned on a new vaccine — not yet licensed, but described by WHO as “safe and protective” — which has so far been used to immunize more than 60,000 people deemed most at risk of infection.
But one key group is denied access: Since the vaccine has not been tested for use during pregnancy, it is not being offered to pregnant women.
“The cost of doing this research versus the cost of essentially denying women access to something that could be highly beneficial, there's really no comparison.”
— Carleigh Krubiner, policy fellow, Center for Global Development and report co-authorCarleigh Krubiner, a policy fellow at the Center for Global Development and one of the lead authors of a recent report on maternal immunization, noted that pregnant and breastfeeding women are often at greater risk of exposure to the virus, because of caregiving responsibilities and proximity with children. “There's significant fear that's been documented among women [in DRC] who are unable to receive the vaccine and know they're at disproportionate risk of exposure just given some of the social roles,” she told Devex.
This has left women and the babies they carry unprotected from a virus that kills around half of everyone who contracts it. It has also reduced the overall population-level immunity, leaving gaps in ring vaccination efforts that target those most likely to become infected.
It is a common situation during outbreaks and epidemics. Most live vaccines are not offered during pregnancy due to a lack of evidence about how they might affect the fetus, since pregnant women are almost always left out of clinical research in developing epidemic vaccines. While there are good reasons to be cautious about how they are included in some types of research, Krubiner explained, excluding them ultimately exposes them to greater risks when outbreaks hit.
The new report, supported by the Wellcome Trust, offers guidance on when and how to include pregnant women in vaccinations against emerging epidemic threats. The authors note that pregnant women often suffer “disproportionate risks” from exposure to these viruses, yet “widespread failure to appropriately include pregnant women in vaccine research means that ... in numerous outbreaks and epidemics, pregnant women have been denied opportunities to receive vaccines that would have protected them and their offspring from the ravages of these diseases.”
Even as recently as the West Africa Ebola outbreak of 2014-2016, opportunities to “gather more robust data on pregnancy,” which could have helped to protect pregnant women the next time around, were missed, Krubiner said.
“There were recommendations to include pregnant women in those trials, especially given the risk-benefit calculus at the time, and ultimately for a whole host of reasons those recommendations were not taken up,” she said. “The cost of doing this research versus the cost of essentially denying women access to something that could be highly beneficial, there's really no comparison. We can't afford to leave this group unprotected.”
In the past, women and children more broadly were excluded from clinical research over fears for their safety. But a growing recognition of the risks this created meant that, since the 1990s, the United States government has insisted any medical research it funds must include women and minorities.
Krubiner believes the inclusion of pregnant women must now also be incentivized. For example, she suggested that requests for proposals and funding announcements for new products could include requirements to generate evidence on use during pregnancy. That would help lay the groundwork for further research down the line and “signal to researchers [and] policymakers that this is the direction that epidemic response and vaccination needs to move in.”
The report adds that there should be a “presumption of inclusion” of pregnant women in vaccine trials and campaigns unless there are specific scientific or ethical reasons to leave them out.
“The development community [as funders and advocates] really does hold a lot of power to reshape the agenda in a way that is much more inclusive to address the needs of pregnant women and their babies,” Krubiner said.
While a small but rising number of vaccines are now being developed specifically for use during pregnancy, pregnant women are still rarely included in the development of vaccines targeted at more general populations. But with increasing attention being paid to vaccine research for epidemics — through initiatives such as the Coalition for Epidemic Preparedness Innovations, a public-private coalition that aims to speed up vaccine research, and WHO’s blueprint for research and development — there is an opportunity for change, Krubiner said.
“There's a lot of effort right now to try and bring to market new and innovative vaccines so that the next time there is an outbreak of Lassa fever or Nipah virus or even Ebola we will have more tools at our disposal … All of those efforts that are happening now can be leveraged to proactively include pregnant women in the response,” she said.
“I think we have a moment right now to learn from our past failures and to really change, to shift the paradigm.”








