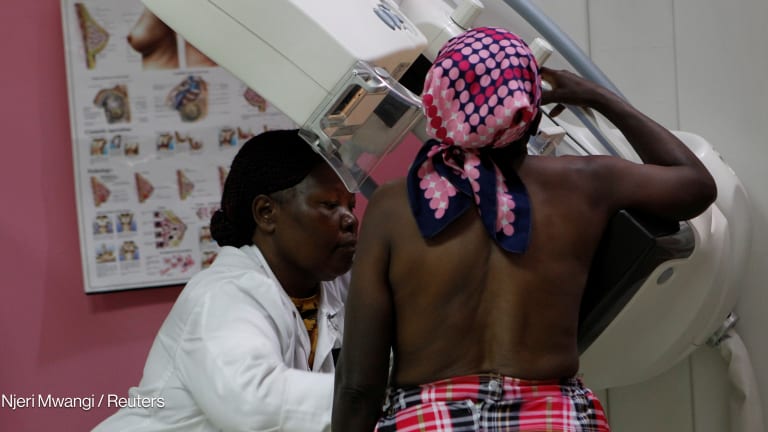
There have been significant advances and developments in global health over the past decade.
According to the World Health Organization, there are now more children living longer lives than there were 20 years ago, maternal deaths have been decreasing steadily, and 1 million fewer people contracted HIV in 2013 than in 2001.
Even so many people, especially in low-income nations, still die from curable and preventable diseases, including diarrhea and road injuries — which WHO projects would be some of the leading causes of death in the next 15 years. Many more are dying without even receiving medical attention or knowing what caused their deaths.
Printing articles to share with others is a breach of our terms and conditions and copyright policy. Please use the sharing options on the left side of the article. Devex Pro members may share up to 10 articles per month using the Pro share tool ( ).
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5