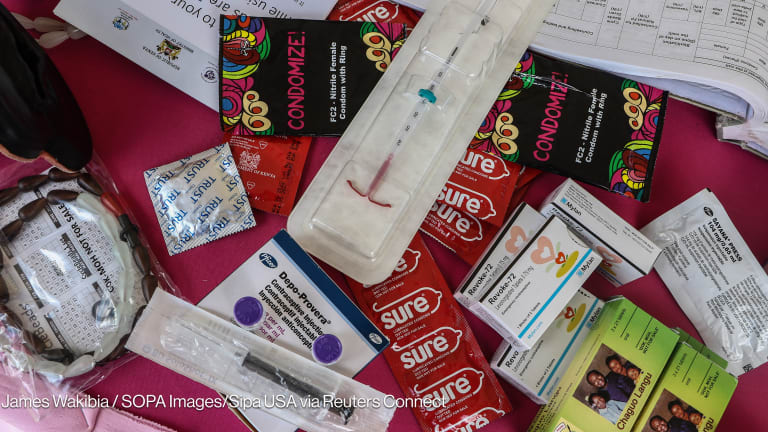
Unintended pregnancies take a harrowing toll on women, young people, families and nations. When women are unable to decide whether and when to have children, maternal and newborn deaths rise, educational and economic opportunities are lost, families, communities and countries suffer greatly.
Global data highlights the tremendous challenge we face: 213 million pregnancies occur annually and an astonishing 40 percent — about 85 million — of these are unintended. In the United States alone, there are approximately 3 million unintended pregnancies each year, and in India, a staggering 18 million. A woman’s ability to make informed decisions about her reproductive health is one of the most basic human rights. It is a decision that can determine what kind of future she will have — and whether she will have one at all.
Emergency contraception is a unique tool for women to space and time their pregnancies. It is grossly underutilized, underfunded, and not fully optimized globally. It is the only contraceptive method that can be taken after unprotected sex and is effective for several days to prevent pregnancy. It is especially needed by women who have been sexually assaulted, who are often desperate to avoid becoming pregnant by their rapist.
One thing to be clear about, since misinformation abounds: Emergency contraception is not abortion and should not be confused with medical abortion drugs. If a woman has already become pregnant, the EC pill will have no effect. It also will not prevent a fertilized egg from implanting into the uterus.
EC serves as a backup for broken condoms, unplanned sex, and mistakes made with fertility awareness birth control. It could meet the needs of millions of women who are not currently using contraception. The method is safe, suitable for all women, backed by a slew of evidence, and yet remains largely unheard of by millions of women and their partners. Positive disruption, support and creative thinking are urgently needed to ignite action on this issue.
More than 200 million women in developing countries currently have an unmet need for family planning; they want to avoid pregnancy but aren’t using a modern method of contraception. According to a recent report from the Guttmacher Institute, one of the most commonly cited reasons is infrequent sex.
For women whose husbands are away or whose sexual relationships are sporadic, a long-term contraceptive method may not make sense. Using EC on an as-needed basis gives these women another way to protect themselves. EC can fill an important gap, making more contraception options and choices available to more women.
So why doesn’t EC figure more prominently in family planning programs worldwide?
One reason may have to do with the way contraceptive methods are pigeonholed. EC is often regarded as a method provided by the private sector, in pharmacies, rather than through regular family planning programs. Another challenge is the concern that offering women the option of choosing less effective methods may deter them from using highly effective ones, such as IUDs or implants. Finally, EC is seen primarily as a part of sexual assault services, not family planning.
The World Health Organization’s guidelines include EC as an essential intervention after sexual assault. In crisis zones, with heightened levels of sexual violence, EC is routinely included in emergency supply kits. Many donors and public health professionals are accustomed to thinking of EC primarily in these contexts.
Brave advocates, family planning professionals, and some innovative foundation funders have worked hard to put EC on the map over the last two decades, bringing the product through the regulatory process, piloting EC in selected countries, and building up the scientific evidence and programmatic experience necessary to make this critical family planning method available worldwide.
Despite these good intentions and actions, the family planning community has failed to provide adequate support for and information about this game-changing contraceptive method. The majority of women and girls in developing countries don’t even know that emergency contraception exists.
In Africa, the percentage of women who have heard of EC ranges from 5.7 percent in Chad to 59.2 percent in Kenya. For those who have information about EC, they may be prevented from access because it is cost prohibitive. Since EC is largely provided by the private sector, prices range widely: from $2 to $8 a dose in the Democratic Republic of the Congo to $50 in the United States, making it unaffordable and far from reach for large segments of the population, especially the most vulnerable and marginalized women and girls.
The government in the DRC strongly supports family planning and pledged to raise the country’s contraceptive prevalence rate to 19 percent by 2020. The pledge forms part of its commitment to Family Planning 2020, a global partnership to provide 120 million additional women and girls access to lifesaving contraceptives by the year 2020. There is strong domestic and international donor commitment to expand access to contraception. Emergency contraception has been on the DRC’s list of essential medicines since 2010, and is supposed to be available by prescription at public health centers.
Challenges abound; one study of 21 public health centers found that none of them had EC in stock. It is not widely integrated into family planning systems, and brochures created to explain contraceptive methods to women did not include any information on EC. Most of the country’s EC is shipped as part of emergency kits to the conflict zones in eastern Congo, where rape is endemic.
There is a tremendous opportunity in the DRC to emphasize EC more in the public and private sector. Partnerships with NGOS are critical to driving transformational change. DKT, a social marketing organization, has just introduced the Aleze brand of EC to be sold in drugstores and pharmacies. At the same time, government officials are interested in the integration of EC into family planning programs; informational materials on EC for family planning clients are under development, policies are being updated, and plans are underway for EC to be more consistently available in family planning clinics. The potential for impact is enormous: DRC has one of the lowest contraceptive prevalence rates in the world — just 8 percent of women are using modern contraception — yet women there express a strong desire to space their childbearing (45 percent of women) or have reached their desired family size (23 percent of women). However, the latest surveys show that only 18.8 percent of women have heard of EC. That is bound to change for the better as DKT markets its products and the government ramps up its efforts to make EC information and access more widely available.
So how can we collectively accelerate women’s access to this critical technology?
The family planning community must pick up the momentum and work to integrate EC into family planning services, discussions and country plans. Donors must consider funding programs that include EC as part of the contraceptive method mix. More research and testing are needed to understand whether community-based distribution systems can successfully and safely provide EC. Data collection also remains a challenge, though the community is beginning to address this with the inclusion of a question related to EC use in the Demographic and Health Surveys in 2014. New mobile data collection programs such as PMA2020 will also gather more frequent data about women’s contraceptive use.
We have a tremendous opportunity to elevate emergency contraception as a critical pathway to meet the needs of women and youth, promote informed choice, and support countries’ family planning goals, especially as we mark the midpoint of the Family Planning 2020 initiative, a significant milestone on the journey to realizing the Sustainable Development Goals, and contraceptive access for all, by 2030.
An important gathering of experts takes place on Sept. 21-22 in Washington, D.C., where conversations will be held on topics such as EC in community-based distribution, new channels of availability including in online access, and high prices in pharmacies. Co-sponsored by the International Consortium for Emergency Contraception and the American Society for Emergency Contraception, the EC Jamboree is an annual conference that brings together an international group of public health experts to share research and information on EC, discuss strategies and identify action plans for improving access.
EC is one of a kind. It remains the only contraceptive method that is effective after sexual intercourse, and is one of the most underutilized tools to broaden access and choice for women and youth globally. Governments, civil society, the private sector and NGOs all have a role to play in making sure that EC is widely accessible, integrated into the mainstream, and available to every woman and girl who wants and needs it.
Ultimately, women and girls deserve to have effective methods, full information, and affordable and quality products to plan their families and their futures. It’s up to all of us to ensure this “best-kept secret” doesn’t remain a secret any longer.
For more Devex coverage on global health, visit Focus On: Global Health