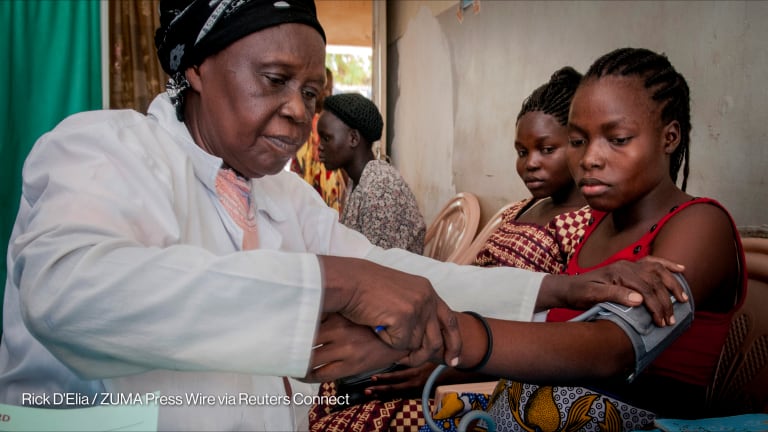Opinion: We need a Marshall Plan to train health care workers around the globe

As the United Nations General Assembly kicks off, leaders from around the world are gathering in New York for a high-level meeting focused on universal health coverage.
Their mission: to determine how governments and donors can best achieve the U.N.’s Sustainable Development Goal on universal health coverage (SDG 3.8), which states that, by 2030, “all people and communities receive the quality health services they need, without financial hardship.” This is both a lofty goal and a worthy one. But in order to realistically achieve it, we must address an emerging crisis: the rising shortage of health care workers around the globe.
Training new health care workers does not have the cachet of eradicating malaria or finding a cure for cancer. But if we really want to ensure that all people have access to the quality health care they need and deserve, this is the single most important thing we should commit to achieving over the next decade.
Ahead of the meeting, UHC2030 mapped out the specific steps we must take to achieve universal health coverage. Included among them is training “a health workforce based on quality and competence, with a special focus on nurses, midwives and community health workers.” This vital frontline workforce will comprise tens of millions of new workers around the world — and if we do it sustainably, we can ensure qualified health workers for generations to come.
Unfortunately, we are currently headed in the opposite direction. By some estimates the worldwide shortage of health care workers will reach 15 million by 2030. In countries such as Syria and Venezuela, thousands of doctors and nurses have fled violence and instability. In Sierra Leone, 21% of the medical workforce died in the 2014 Ebola epidemic. And countries that boast significant numbers of trained professionals — the Philippines, for example — see many of them leave to practice elsewhere.
The World Health Organization reports that there has been a 60% rise in the number of migrant doctors and nurses working in Organisation for Economic Co-operation and Development countries over the past decade. This helps with immediate health needs in many places, but it is not a long-term, sustainable solution. We don’t necessarily need to move health care workers around the globe; we need to train more of them, everywhere.
International NGOs must see it as our duty not only to provide aid, but also to transfer skills and knowledge so that people become agents of their own good health — and their community’s health. We must focus on building health systems in every country and then training people locally — the people who know their communities best — to address their community’s health challenges.
I recently visited two hospitals in the Dominican Republic where my organization, Project HOPE, is helping train health care workers. When we first started working there, we met doctors and nurses who weren’t properly trained to identify and address stress factors in mothers and babies. They were working with a severe shortage of equipment — two or three babies crowded into one incubator, and makeshift oxygen masks crafted from water containers.
Project HOPE equips these hospitals with newborn intensive care units. But we also train doctors and nurses to utilize those NICUs to save lives, and to teach parents how to care for their children in the vital first 30 days of life. In just one year, we have seen a drop in both maternal and infant mortality.
This is just one example of how training health care workers to provide care in their own communities can have an enormous impact. In Mali, an initiative to provide free door-to-door health care visits for pregnant mothers and young children has contributed to a dramatic drop in child mortality rates. And governments from Ethiopia to Malawi have made dedicated commitments to increasing the number of local health care workers in their countries.
Spending donor dollars on training workers has an exponentially greater impact than spending money directly on treatment, because these workers will go on to provide care in their communities for many years to come — and they will also train others. It means better health outcomes, stronger communities, increased economic growth, and greater empowerment for women, who make up much of the world’s health workforce. Indeed, the High-Level Commission on Health Employment and Economic Growth asserts a return on investment in health at a ratio of 9:1.
Consider Africa, where on parts of the continent children can contract malaria as many as seven times per year. Unable to send their children to school, parents miss up to five days of work every time their child gets the infection. For many people, these missed workdays may mean the difference between feeding their families, or their children going hungry. A trained workforce of local doctors and nurses can treat those patients immediately and create a positive ripple effect in their community. Moreover, considering that two-thirds of health care workers worldwide are women, more training also means increased potential for more women to earn a living and support their families.
For all of these reasons, we need governments and donors to commit to a Marshall Plan for training health care workers across the globe. In the same way the Marshall Plan spurred European recovery following World War II, we must see a global health workforce as an investment worth championing.
All U.N. member countries have already committed to achieving universal health coverage by 2030. Yet to date, the approach to tackling this issue has been disjointed. Certainly there is important work being done, but it is too sporadic and not well coordinated. It is usually based on a donor being exposed to one issue in one country and committing to addressing that issue.
Instead, we need a coordinated global effort to train health care workers and expand their knowledge and skills, especially nurses, midwives, and community health workers who can play a vital role in diagnosing and treating illnesses in places where doctors are few.
When the high-level U.N. meeting wraps, I hope to see specific commitments about how many health care workers will be trained over the next decade, and how this vital mission will be funded. Addressing this shortage is the most pressing public health challenge facing the world today. It is high time for all of us to rise to it.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5