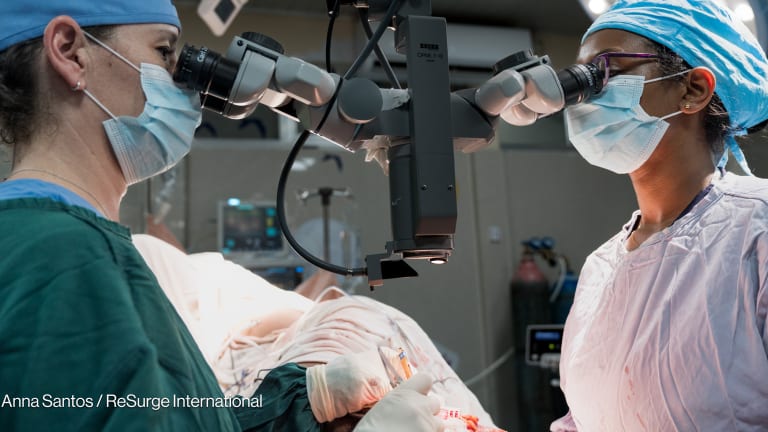
One year on: Is Africa’s surgical equity push delivering real change?
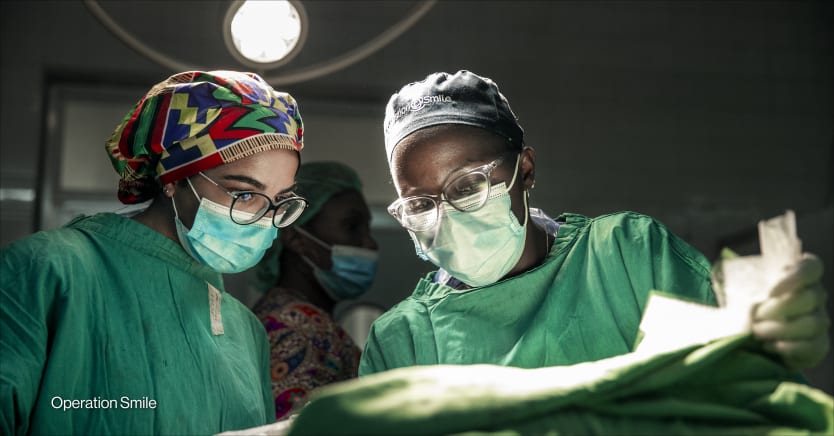
One year after the inaugural Pan-African Surgical Conference, health leaders gathered virtually for what they described as an accountability moment.
In a discussion hosted by Devex in partnership with Operation Smile, they sought to answer a key question: Have commitments to strengthen surgical systems across Africa translated into concrete policy shifts and measurable progress?
Globally, five billion people lack access to safe, timely, and affordable surgical care. Each year, at least 77 million disability-adjusted life years could be averted through basic surgical services. In many low- and middle-income countries, distance, fragile infrastructure, and severe workforce shortages continue to keep essential surgery out of reach.
Against this backdrop, panelists focused less on pledges and more on implementation — and on what it takes to localize surgical access in ways that endure.
National ownership drives sustainability
Professor Faustin Ntirenganya, chair of the surgery department at the University of Rwanda and cochair of the Pan-African Surgical Conference, described the past year as one of growing continental collaboration.
“[Before the conference] I knew a few African surgeons, but after the conference, we became a big village. … We realized we have a lot to share,” Ntirenganya said.
Cross-border exchanges and emerging surgical networks are strengthening capacity across Africa. But long-term impact, Ntirenganya emphasized, depends on political ownership.
“This is an African issue, which should be owned by Africans. … This is the only way things are going to be sustainable,” he said.
Building local surgical teams is essential
For decades, Operation Smile has expanded access to cleft surgery through locally led surgical programs and global partnerships — always with a focus on strengthening the health systems where it operates. That commitment continues, said Dr. Elizabeth Coté, senior vice president of global programs at the nonprofit, but experience has underscored the importance of expanding even further, particularly to district hospitals closer to where patients live.
To advance this work, the organization has launched Operation 100, a bold commitment to equip district hospitals with essential tools — from reliable oxygen to safe anesthesia equipment — while training full surgical teams, not just individual surgeons. The goal is to bring safe surgery within two hours of patients’ homes whenever possible. “Then, care can be delivered where people need it, when people need it, by their own neighbors and the professionals in their own neighborhoods,” Coté said.
By investing in both people and infrastructure, these efforts build stronger health systems and ensure sustainable access to a wider range of essential procedures for years to come.
Harmonization strengthens workforce capacity
Expanding the surgical workforce requires more than increasing enrollment, said Stella Itungu, chief executive officer of the College of Surgeons of East, Central, and Southern Africa, or COSECSA.
Operating across 24 countries, COSECSA faces limited training capacity and fragmented regulatory systems that slow scale. To address those constraints, regional leaders have worked to align accreditation and training standards across borders so that “one curriculum works across the region,” Itungu said. That harmonization and standardization of qualifications, she added, has helped streamline many of the challenges the region faces, particularly workforce shortages.
The path forward
Panelists pointed to stronger professional networks, expanded district-level capacity, and growing policy alignment. The true test, they agreed, is whether those reforms translate into patients accessing safe surgery close to home — reliably, affordably, and without delay.
If surgery is to be treated as a basic human right, locally led systems must be backed by sustained financing, workforce investment, and long-term leadership. Without that follow-through, progress risks remain fragmented — leaving millions without access to lifesaving care.
The next phase of surgical equity will hinge on whether governments and donors convert collaboration into durable systems — financing the training, infrastructure, and governance reforms required to make locally led care the norm rather than the exception.
Watch “Beyond the promise: Tracking progress and policy shifts for surgical equity in Africa” here.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5