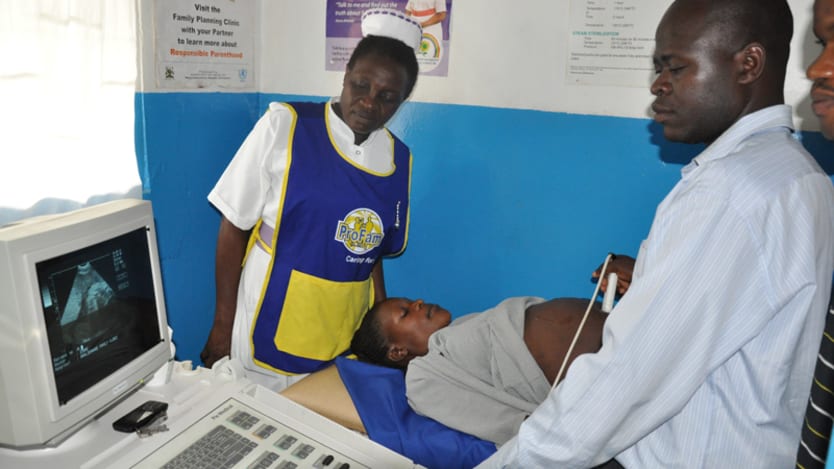
One day in September, in a small town north of Kampala in Uganda, a young woman, pregnant with twins and still weeks away from full term, arrived at the Maria Maternity Ward, a private clinic. Her cervix was already 8 centimeters dilated. The babies were coming.
Midwife Mary Gorret Musoke knew what to do. She monitored her patient’s blood pressure and prepared her for the premature delivery. She called a doctor she knew, who gave her some advice on how to give the imminent newborns and their underdeveloped lungs a fighting chance.
“The babies came,” Musoke recalls with a smile, “and I did the kangaroo wrap — one with the mother, one with the father.”
Today, all are healthy and thriving.
The case could have gone very differently. The mother could have attempted to deliver at home, a risky proposition that remains far too common in this part of the world. She could have set out for the public district hospital in the city much farther away, a facility Musoke, who used to work there, says is so overcrowded and understaffed at times that many women end up delivering alone on the floor. Instead, she chose “Mama Maria.”
Maternal health issues 'aren't finished yet' — and neither is Jill Sheffield
Jill Sheffield will step down as president of Women Deliver after the organization's fourth global conference on the health and well-being of girls and women. Devex caught up with Sheffield on what's motivated her as a champion of women's health for more than 40 years — and what attendees can expect at May's conference.
That an increasing number of women from Musoke’s community and surrounding villages are making that same choice is a testament to the midwife’s success as a private maternity care provider as well as an entrepreneur. When Musoke first started out in private practice — after resigning from her district hospital job, frustrated with the public facility’s lack of resources and a recognition that her community needed her closer by — she delivered a few babies a month in her sitting room.
Today she takes care of more than 110 patients a week, operating a facility with three beds, a separate exam room and a staff of five offering a full menu of maternal and reproductive health services, from labor and delivery to antenatal care and postpartum family planning.
Thanks to the training and other support provided by Population Services International through PACE, PSI’s local affiliate, a partner in the MSD for Ugandan Mothers program, Musoke acquired the additional clinical expertise she needed to handle high-risk cases with confidence. She knows how to manage excessive bleeding and screen for signs of complications. She has an ultrasound machine and an autoclave for sterilizing equipment and preventing infection, investments that help set her clinic apart. She’s up on the latest protocols and safety checklists, and she knows her limits: the doctor who was once her mentor is now a regular source of consults and referrals.
And by taking a separate course in business management, also through PACE, Musoke learned a whole set of other “tricks” she says have been essential to making her clinic sustainable: keeping the books, watching her costs, hiring a receptionist and finding other sources of revenue, such as selling contraceptives and other commodities, to help keep her enterprise afloat so she can continue serving women while also make a living.
That’s not easy to do where so many live in poverty. Musoke treats many women for free, those she knows are too poor to pay, and she says they compensate her by referring their friends. Free exercise classes for pregnant ladies also help attract new clientele.
Arming providers such as Musoke with the clinical skills they need to deliver quality care as well as the business management skills they need to thrive as independent operators is one of the most effective ways for a country such as Uganda to strengthen its maternal health system and reduce maternal mortality. While it’s important to continue efforts to improve public health systems, country governments, with help from the donor community, must also look to private providers to do their part to bring affordable, high-quality care to women in underserved communities.
The fact is, the private sector already plays a prominent role in maternal health across the developing world. Roughly 40 percent of women who receive care — rich and poor — receive private care, according to a recent London School of Hygiene and Tropical Medicine analysis.* And the Results for Development Institute’s Center for Health Market Innovations has documented hundreds of examples of private health care providers delivering high-quality care. Yet the private sector is often overlooked as part of the “formal system,” leaving it largely unregulated and of variable quality.
To address these issues, the global health community must find ways to help governments more effectively engage with private providers and link them to quality of care improvement initiatives. We must help governments build workable payment systems that allow private providers to be reimbursed for their services when patients can’t afford to pay them directly, while making payment contingent on providers meeting and maintaining quality standards.
Through a program backed by the PharmAccess Foundation in Kenya and Nigeria, among other countries, low-cost business loans are made available to private clinics that meet certain accreditation requirements. In Ghana, private care is covered under national health insurance, but only if the provider is government-accredited. The Joint Learning Network for Universal Health Coverage is working to develop better mechanisms for governments to engage private providers and create payment systems that incentivize quality while also making care more affordable.
When given the payment incentives and the proper training and support, we have observed that private providers can and will “step up their game.” Nongovernmental organizations and other donor organizations and professional associations can help drive these activities, by providing support and guidance, and facilitating the sharing of best practices across borders. Social franchising and other models for organizing providers into networks can also help governments monitor performance and exchange information, and get data back that helps them track community health trends.
By providing high quality, personalized care at the community level, Musoke is helping more women survive pregnancy and childbirth. Governments and partners can change the landscape of maternity care by integrating more small-scale providers such as Musoke into the broader health system through payment and quality initiatives that help them provide affordable, quality care to lower-income patients and create sustainable small businesses.
We look forward to discussing the role of private sector providers at Women Deliver, during an MSD for Mothers-sponsored session titled, “Whose Business is it Anyway? Tapping Local Businesses to Improve Maternal Health” on May 17. For more information, visit wd2016.org.
Interested in more stories about women's and girl’s health? Make sure to follow us this May for live Devex coverage of the fourth Women Deliver conference in Copenhagen, Denmark. Join the conversation by tagging @devex and using #WD2016.
* Correction, May 27, 2016: This article has been updated to clarify that roughly 40 percent of women who receive care — rich and poor — receive private care.
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5









