The World Health Organization's reclassification last month of progestogen-only injectable contraceptives has triggered a critical debate in the family planning community over how to manage the potential link between higher rates of HIV acquisition and one of the most popular birth control methods in many at-risk communities.
Reviewing the past 35 years of research, the international health body noted the persistent ambiguity in findings linking injectable progestogen to higher rates of acquiring HIV. WHO reclassified the contraceptive to say its benefits still outweigh any risks, but said “women considering progestogen-only injectables should ... be advised about this, about the uncertainty over a causal relationship, and about how to minimize their risk of acquiring HIV.”
The WHO had previously classified progestogen-only injectables — the most popular of which is depot medroxyprogesterone acetate (DMPA), often marketed as Depo Provera — as safe for everyone.
The change should not affect the availability of Depo or other progestogen-only injectables. In fact, the method may soon become even more accessible and dominant across the developing world, with the likely expansion of a self-injecting formulation of DMPA known as Sayana Press. The method is currently still being evaluated, but backers envision wide distribution.
However, the reclassification should spark new conversations between providers and patients, drafters say. “This decision foregrounds women's right to have all the information, including this potential risk, so they can make a choice,” said Emily Bass, the director for strategy and content at AVAC, an HIV prevention advocacy group, and a member of the guideline development group the WHO assembled to consider the reclassification.
Providers said the new guidance is causing them to rethink how to identify a woman with a higher likelihood of acquiring HIV and how to communicate the possible risk of the injectables to those clients. The stakes are enormous: Depo or other progestogen-only injectables are among the most widely available family planning methods in many communities where HIV transmission rates remain high.
Among some HIV prevention advocates, the impulse is to do whatever is necessary to limit even a possible risk of increased acquisition — even if that goes beyond the WHO guidance. The family planning community, while deeply concerned about women's health, is also protective of gains it has made in recent years. Though the ultimate goal of both groups is protecting women's health, there is some tension over how best to convey the new guidance.
Prevalence of injectable contraceptives in sub-Saharan Africa
In many areas of sub-Saharan Africa, an injectable contraceptive is often seen as the easiest option for women — if not the only one. Injected just once every three months, it is far more discreet than pills or a condom, which is important in societies where contraceptive use is still stigmatized. Other options, such as long-lasting implants or copper intrauterine devices (IUDs), which involve inserting something into a woman's body, can raise questions among clients that overstretched health workers may not have the time or training to answer.
That popularity is met out in the numbers. Injectables are the most common contraceptive in 27 of the 69 mostly-developing countries where the global partnership Family Planning 2020 focuses. In four countries where UNAIDS has recorded an HIV prevalence above 2 percent, FP2020 reports that injectables make up between 50 and 60 percent of the contraceptives used — Uganda, Rwanda, Malawi and Chad.
Until now the accessibility and ease of injectables has mostly overshadowed the persistent questions over whether they, and other hormonal contraceptives, increase a woman's risk of acquiring HIV.
In Uganda, many health providers at government clinics are almost unaware of the growing concerns about whether Depo usage increases the risk of HIV acquisition, said Dr. Carole Sekimpi, the managing director for Marie Stopes Uganda. Depo represents only a small percentage of the contraceptives her organization provides, she said.
“The population doesn't know what to demand for,” Sekimpi said. “They are not demanding for what they should because they don't get the right counseling.”
New WHO guidance
WHO’s new guidance was aimed at improving women’s understanding of possible risks, Bass said. “The motivation was to make sure that women get this information,” she said. “That they understand it's not proven, but it's a possibility.”
The challenge for providers is how to convey that information without alienating or discouraging women from using contraceptives, particularly in cases where there are few options available.
“I don't think there is a great, clear answer of how you communicate it,” said E. Tyler Crone, coordinating director of the ATHENA Network, which seeks to improve gender equity and human rights coverage in the HIV response. “You say, 'Here's this contraceptive method, but it might make you more vulnerable to HIV.' It's putting women in an impossible scenario.”
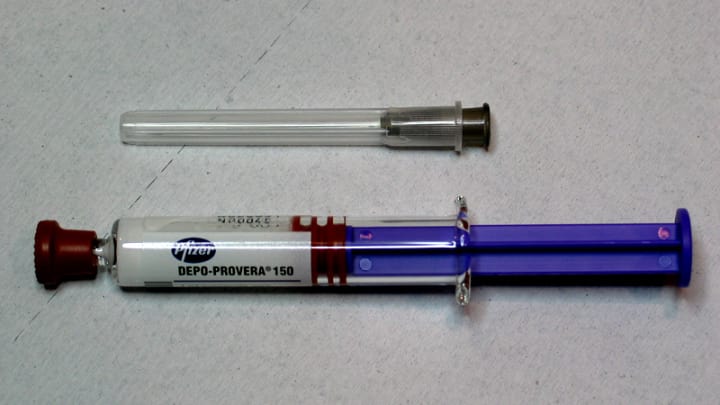
The situation will become more complicated with the likely expansion of Sayana Press. Unlike Depo and other progestogen-only injectables, which require a muscular injection, Sayana Press is effective with a lower dose administered subcutaneously. Packaged in a kit along with a needle, women can easily be trained to inject themselves. Studies are underway to determine its effectiveness, though there are already expectations it could dramatically expand the reach of family planning.
The Gates Foundation has been a major backer of Sayana Press and orchestrated an arrangement that reduced the price per dose to $1. The group did not respond to specific questions about whether the new guidance would affect their support for the method, though they did offer a general comment that: “WHO's current statements on this revision also reinforce that DMPA, including Sayana Press, can continue to be provided to all women who choose to use it ... regardless of their risk of HIV acquisition.”
Nina Hasen, the director of HIV and TB programs at PSI, agreed that the reclassification presents a challenge to her organization and other providers. For more than three decades and now in more than 30 countries, PSI has been pushing for improved access to a broad range of family planning options.
Hasen, whose comes from a background in HIV programming, said the HIV community has to work with their family planning counterparts to figure out how to classify a woman's risk of acquiring the disease, and to ensure she understands the range of options that are available to her.
“Let's not miss an opportunity to improve our ability here to get serious about what informed choice means and to get together on that,” she said.
Sekimpi envisions something like a checklist of questions health workers could ask of clients, which would then guide them into making suggestions for which family planning methods might be most suitable for her.
What is most critical is that women are fully informed of all of their options and, should a patient express interest in an injectable method, she “should be advised in a wholly respectful, non-judgmental routine way, of the possibility of associated risk,” according to a Civil Society Advocacy Working Group on Hormonal Contraception and HIV. The group, with representatives from nine high-burden HIV African countries as well as Western advocacy groups, said the new guidance would require a greater synthesis between HIV and family planning programs until more information is available.
Diversifying family planning options
An open-label randomized clinical trial is currently underway to determine, among other issues, whether there is a indeed a link between DMPA and increased HIV acquisition. Results are not expected until 2019, so there is likely to be ambiguity in the epidemiological evidence at least until then. Prior to the ongoing study, the most recent systemic review of the available epidemiological evidence, published last year, concluded that “new information increases concerns about DMPA and HIV acquisition risk in women.”
WHO convened a Guideline Development Group on the topic in the absence of a definitive answer. The group, which met in Dec. 2016, included experts in family planning and HIV, researchers, and representatives from affected populations.
Activists said they hope the reclassification pushes governments and donors to diversify family planning options so that women, once they are fully informed, have a choice beyond Depo, condoms or nothing at all.
“Choice is only possible if there are other things on the shelf,” Bass said.
For this to happen, Sekimpi said, health workers need to inform clients about additional methods so they know to ask for them. Once they start to issue the demand, she said donors and governments would likely respond.
But it will likely also require high-level lobbying, to ensure donors are funding a variety of methods, and that governments are willing to stock them. More complex interventions, including implants or IUDs, will require more and better equipped facilities and trained health workers.
“We're going to be watching whether this takes care of the right to information and the right to choice,” Bass said.
For more Devex coverage on global health, visit Focus On: Global Health

