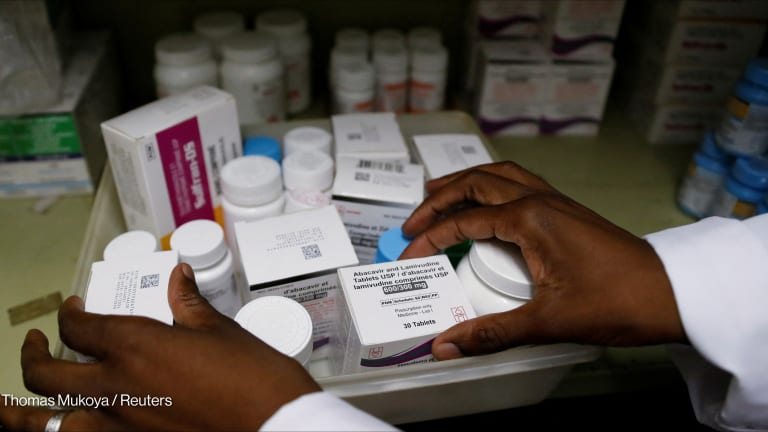
Opinion: Weak health systems kill — here's how we can stop that from happening

Community health workers, or CHWs, are an important part of the primary health care system. They can reduce child morbidity and child mortality and ultimately create a return on investment with a ratio of up to 10 to 1.
During this pandemic, interest in community-based approaches has increased: Every nation that has dramatically slowed the rate of COVID-19 infection has done so through aggressive community testing and contact tracing, and calls for the creation or strengthening of national CHW programs have been published from the U.K. and the U.S. to India.
With attacks against health workers on the rise, advocates call for action
“We see a lot of talk [about how to tackle violence against health workers] ... but we don’t really see that much action on the ground," says ICRC's Maciej Polkowski.
But some programs fail to achieve the expected health and economic impact. Even when countries choose to invest in creating or reforming CHW programs, they struggle to set CHWs up for success. Without good design, health systems are less resilient during crises, allowing pandemics to take hold and often leading to declines in utilization of essential health services — which can ultimately kill more people than a pandemic itself.
Luckily, this is not inevitable. By using a well-established, evidence-based tool — the Community Health Worker Assessment and Improvement Matrix — we can design and invest in high-performing CHW programs during and after this outbreak.
There are 10 components of the toolkit that ensure community health systems can implement to not simply beat COVID-19, but emerge stronger.
1. Roles and recruitment
Recognize CHWs as part of a country's coronavirus response, include them in projections for personal protective equipment and essential supplies, and modify their tasks as required. Existing CHW networks can facilitate a rapid response while new CHWs are recruited and trained. After civil society made the case to the Kenyan Senate for instance, the country now includes CHWs in national PPE estimates.
2. Training
Leverage existing digital technology and e-learning platforms to train CHWs and provide continual, remote training, especially when in-person training is not possible and protocols are changing quickly. VillageReach is working with Viamo in Mozambique and the Democratic Republic of the Congo to train CHWs on COVID-19 curricula using interactive voice response messaging on basic phones, while Medic Mobile has built modular text-messaging and app-based tools powered by the Community Health Toolkit.
3. Accreditation
Administer post-training tests to ensure CHWs possess the knowledge and competencies required to protect themselves while delivering quality patient care. As part of Liberia's National Community Health Assistant Program, the Ministry of Health is administering pre- and post-training tests as part of the coronavirus training package to assess knowledge and ensure CHWs are appropriately prepared to provide care at the community level.
4. Equipment and supplies
Integrate CHW supply needs with national supply plans so quantification, distribution, and financing support all cadres of health workers, especially PPE for CHWs, which is currently inadequate. One to One Africa in South Africa and Lwala in Kenya have provided national coordinating bodies with catchment and county-level data to improve precision of national estimates.
5. Supervision
Ensure CHWs are paired with a dedicated supervisor — which is critical as professional protocols evolve and health and safety risks increase. Support supervisors to review summary statistics of CHW performance, assess patient experience, and support CHWs remotely. Living Goods, for example, has given CHWs additional data and airtime to support phone-based patient contact and remote supervision support.
6. Incentives
Pay CHWs at a competitive rate relative to the respective market consistently, on time, and commensurately with the job. Reallocate money currently earmarked for performance-based incentives to cover routine salaries. Give CHWs hazard pay, and pay for overtime and sick leave. For example, Liberia’s National Community Health Assistant Program pays CHAs a minimum wage in line with the World Health Organization’s CHW guidelines.
7. Community Involvement
Have CHWs engage in socially distanced community dialogue about preventing, detecting, and responding to the pandemic, and support CHWs to channel feedback to the health system. CHWs in Togo have been trained by Integrate on COVID-19 information and given informational posters to engage in socially distanced community education.
8. Advancement
Offer professional advancement opportunities to recognize and reward high-performing CHWs who go above and beyond during the pandemic. In Mali, Muso promotes high-performing CHWs to dedicated supervisors.
9. Data
Ensure CHWs document their visits consistently in a standardized format and report data to public sector monitoring and evaluation and logistics management information systems. CommCare, Community Health Toolkit, and others have apps being used from Kenya to Madagascar that allow CHWs to self-check before visiting households and report household data and any emerging cases.
10. Integration into the national health system
Recognize CHWs as part of the formal health system who can identify cases, perform contact tracing, and refer patients to health facilities to receive timely clinical care. For instance, the ministries of health in Kenya, Uganda, and Liberia have incorporated CHWs as part of the coronavirus response, including community awareness raising and contact tracing.
Governments across the world are currently working overtime to respond to COVID-19. Luckily, the investments necessary for rapid community response in an epidemic are the same as those required to prevent the next pandemic. If we support CHWs across these 10 key areas, we will protect them, interrupt the virus, maintain health care services, shield the most vulnerable, and lay the groundwork for better health for all.
Visit the Duty of Care series for more coverage on how health systems can function better so that health care workers are supported and protected. You can join the conversation using the hashtag #DutyOfCare.

Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5