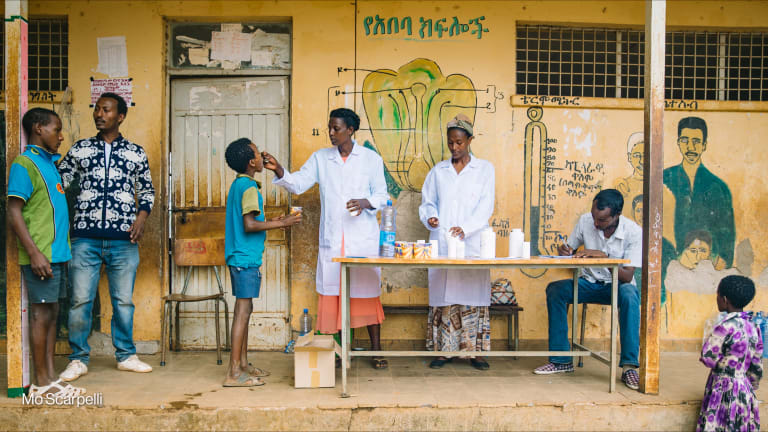
Q&A: What needs to be done to eliminate river blindness in Africa

ABU DHABI — They are two diseases with two different parasites. So for decades, river blindness and lymphatic filariasis have been combatted separately, through different treatment campaigns and by different health organizations and initiatives.
Nothing would be peculiar about this, except that the two diseases actually respond to the same single drug, Ivermectin (also called Mectizan), and are both often found in the same, riverside communities. “It’s about time” to treat them together, the Carter Center’s Frank O. Richards and two co-authors wrote in The Lancet two years ago.
Now that notion is a bit closer to reality with the launch this week of a $100 million joint Reaching the Last Mile Fund to tackle the two diseases through single interventions with a combination drug therapy.
“I think it’s really great that the LF and river blindness programs are being spoken to in the same breath in this initiative,” Richards told Devex. We can “fight both diseases at once, with one round of treatment. That’s not happening, and that needs to stop.”
Richards, who directs the Carter Center’s river blindness, lymphatic filariasis, schistosomiasis, and malaria programs, previously served as a river blindness officer for the U.S. Centers for Disease Control and Prevention in Guatemala, one of six countries in the Americas to have endemic river blindness.
Last year, he watched as that country celebrated elimination of the disease — a feat he now hopes can be replicated in Africa, where the most cases are found.
Now Richards sees elimination in sight. Drawing on the lessons from successful past eradication, his long-term expertise in helping orchestrate a drug donation program from pharmaceutical company Merck, and the political and financial push announced in Abu Dhabi, he told Devex how a successful last mile push could look. The conversation has been edited for length and clarity.
How have you watched the fight against river blindness evolve over the years, and how have we gotten closer to the point of elimination?
Back in 1982 or 1983, I was following with great interest the clinical trials of what was then called MK933, which was Ivermectin. In 1987, when the medicine was donated by Merck — as much as necessary and long as necessary — to fight river blindness, I was stationed by CDC in Guatemala.
River Blindness came from Africa to the Americas largely as a result of the African-Atlantic slave trade. It has such a complicated transmission cycle, that requires a certain kind of blackfly, and so this parasite really wasn’t used to being in the Americas, but nevertheless it established itself in six countries. When I went to Guatemala in 1987, there was terrible river blindness. Mexico had been fighting the condition since 1930s, largely by removing the nodules that the worms make under skin surgically. I happened to be there at a great time when we were establishing these treatment programs, and [I became] very interested in the health education campaigns that needed to go along in order to get people to accept this tablet.
Watching through the years, we’re really now in a third generation of people who have been taking these tablets as part of their routine and their lives. The Mectizan program has really expanded in the Americas and in Africa to essentially control the blindness and the skin diseases that river blindness causes.
We are now at a point of moving from control to an elimination point, where you can successfully stop the treatment without a risk of the disease rebounding — the idea that you scale the programs up, and rather than sustaining the programs forever, we’re looking to safely scale the treatments down, and remove them.
One of the great joys of my professional life is that last year in Guatemala, we celebrated the elimination of river blindness from the country. The president of Guatemala was there, the regional director of WHO was there, there was a big celebration in achieving this. Mexico, Colombia, Ecuador have done this. I really think now, we have our opportunity to do the same thing in Africa. We have yet to take a country off the list in Africa, but we’re close. And with generosity of the UAE and other partners like the Gates Foundation and others, I think we really have a hope to do this in the next eight years or so.
In those four countries, what were the components of the programs that made them successful?
You scale the programs up, and rather than sustaining the programs forever, we’re looking to safely scale the treatments down, and remove them.
—The American river blindness programs are quite different from African programs, which have in general used Mectizan as a once per year treatment. In the Americans, we went from the very beginning on an effort to get rid of the parasite once and for all. It may have been because this parasite wasn’t native, it was not firmly established as it was in Africa, but we also used the Mectizan more forcefully, with two-times per year treatments.
In my opinion, that’s what we need to do certainly in a lot of countries in Africa. We need to really push the agenda with the medicine and treat twice per year, and really be able to push this parasite out.
The other thing that is different in the Americas compared with in Africa control program, is that in Africa — being a control program — it was only aimed at areas with the worst river blindness. But there were other areas that had river blindness infections but really not much disease from it. People said, ‘for the moment that’s not urgent, so just leave those from treatment.’ Those are the areas now people recognize that, if we are really going to really eliminate, we also have to treat.
What we have to do before we finish river blindness is treat some additional areas that see river blindness infection, not much morbidity. We need to do that if we really want to get to zero.
You described the successful plan as being a sort of bell curve — scale up treatments and then scale down. At what point do you move toward scaling down?
The optimistic models say that if [we treat] twice per year, you can finish the job in between six to seven years. If we were to get going in all of these places with twice per year treatment, we could anticipate that six to seven years from now, we would be finished. That’s why there’s reason to believe that in eight or nine years, we could be done with this.
It’s scaling up in order to scale down — that’s what we need to do. A lot of places in Africa have done this. The Carter Center has helped Uganda stop treatments in a number of areas there. They have 17 river blindness foci in Uganda, and 15 of them look as though they have eliminated the parasite. There are areas of Sudan and Ethiopia as well.
“We’ve all seen curves — from getting from nearly controlling a disease and then we stop, and suddenly the graph shows a surge again as the disease comes back. That is what we don’t want to see.”
—I think that what we need to do in this initiative [the Reaching the Last Mile Fund] is to celebrate our successes so that people can see it can be done, not just at a country level, but at the [local] level. Even though the whole country isn’t ready, we can say this part of Uganda we’ve done, so people have faith the approach will work.
But still, we’re going to need to go to two times per year in many areas, expand treatments in many areas, scale up, before we’re going to be able to start looking at brisk scaledown, and I think that scaledown is not likely to occur in broad areas of Africa until you start getting to around 2022 or 2023.
How comprehensive is our mapping of river blindness in Africa at the moment? Do we know which areas have high and low morbidity and infection?
The original mapping of Africa for river blindness was to find the worst areas. [The idea was], let’s start in the worst areas and use this medicine to keep from going blind and keep people from having this stigmatizing skin disease, and that makes perfect sense. But as time has gone on, and we’re really getting rid of this, that’s when people said, ‘we’re going to have to double down if our goal is not just to control — and I mean treat forever and never stop — to getting to the point where we can eliminate.’ To do that, we’ve got to do more, before we do less. That’s the challenge right now.
It’s sometimes not very easy to get across to people: why, if you’re doing so well, do you need to scale up and do a bit more before you can do less?
What it really means from a technical perspective is that you're going to have to go and use more sensitive tests to be able to detect those places that need to be treated. When we first started, it was pretty easy: you didn’t need any sophistication, because so many people had terrible blindness and terrible skin disease. But now that we are at the point where it’s almost gone, it’s harder to find.
You have to recognize that if we were to stop the medicine to soon, and there were areas that still had the parasite alive and well, it could begin to reinvade the areas that we’ve left. We’ve all seen curves — from getting from nearly controlling a disease and then we stop, and suddenly the graph shows a surge again as the disease comes back. That is what we don’t want to see. It’s gotten down, but we want to get it down and out.
How do you prevent resurgence in the areas where you have been able to scale down?
WHO has a pretty clear roadmap as to what you need to do to get to elimination. A lot of this was developed in the Americas, but has been successfully tried in Africa as well. What you need to do is prove that it’s not going to come back, first by stopping treatment, and then by maintaining strong surveillance in those areas for three to five years — to make sure that it doesn’t come back in.
Even beyond that, the concern is that if people migrate back from areas that have a lot of people infected, you have a chance of reintroducing the infection. That’s a really big challenge and usually occurs when people are coming from areas as refugees that were unstable and where treatment programs couldn’t take place in the first place. For example in Uganda, it’s a big challenge in one of the last transmission zones in the country in the North that borders with South Sudan. There are now over 1 million refugees in Uganda, many coming from river blindness areas that had not been successfully treated. That is an area that you have to be really worried about and be involved in getting to and treating to prevent the re-establishing of the condition in other parts of the country.
“The very last cases are often taking place in places of instability, political turmoil, internal displacement, or refugee populations and cross border situations. Very often, it’s not a technical issue but a political issue that is the challenge in reaching the last mile.”
—The whole idea of Reaching the Last Mile is that there’s no point in the course of a life of an eradication program when things get easier. When you start and you’re scaling up, it’s tough. When you’re scaling down, it’s tough. And when you think you’ve done it, you have to maintain surveillance, it’s tough there too. It doesn’t ever get easier. And the very last cases are often taking place in places of instability, political turmoil, internal displacement, or refugee populations and cross border situations. Very often, it’s not a technical issue but a political issue that is the challenge in reaching the last mile.
What are some of the things you’ve learned about effective public health messaging?
The interesting thing both in river blindness campaign as well as in the guinea worm campaign is the grassroots involvement in this, which comes largely from effective public health messaging and engaging communities as partners, not just as receptacles.
“The approach has to be to meet people where they are, to respect them, to promote their own dignity in the process and their ability to contribute and be leaders of the process.”
—In river blindness, so much is done by community volunteers who help to distribute the medicines to their friends and neighbors during the course of once or twice a year campaigns. It’s really essential. The approach has to be to meet people where they are, to respect them, to promote their own dignity in the process and their ability to contribute and be leaders of the process.
We’ve mostly discussed river blindness, but what are the additional considerations for tackling LF as well?
When we wrote in The Lancet in 2015, our article talked about the fact that river blindness and LF often occur in the same villages and districts, that the medicine Ivermectin is used to treat both conditions, but that what we’re seeing right now, for so many years, is that these programs are working separately. They are independent of one another, when using same kinds of interventions — mass drug administration. It makes so much sense to work together, but they haven’t. Why they haven’t is multifactorial, but now is a time when they should.
I think it’s really great that the LF and river blindness programs are being spoken to in the same breath in this initiative. To treat both river blindness and LF, all you have to do is add the other tablet and give a little expanded health education message to fight both diseases at once, with one round of treatment. That’s not happening and that needs to stop. I’m very hopeful that part of this focused initiative will help to rectify that problem in Africa.
It’s a lack of coordination, stove piping, and one program here, one program there, and the opportunities for synergy are missed.
Why haven’t we seen a push on these diseases already, if elimination is technically within reach?
The reason they are neglected is because the people who really suffer the most from them have very little voice and are largely on the margins of society. This is the bottom billion — the billion people who live on a dollar a day or less, and have very little to look to for hope in the future.
These conditions don’t kill, but they maim, and they perpetuate this downward spiral of poverty. Poverty leads them to be exposed to these vectors, then they get poorer and more sick and more poor, and it is really something that we have the opportunity to try and help reverse. It’s not as though by getting rid of LF and river blindness we’re going to end extreme poverty. But it is something we can do, and something we’re doing now. I really hope that we’ll continue to invest in what works and try to make these people’s lives just a little better.
Let’s not forget the people for whom this is all supposed to be about: they are not passive receptacles. They are investing to try to make their lives better and we ought to help them do that.
Read more Devex coverage on global health.
Read more Devex coverage:
► New $100M fund to eradicate river blindness and lymphatic filariasis
► Abu Dhabi to launch campaign to reach 'last mile' on preventable disease
► Progress on ending leading cause of blindness at near standstill, report says
Search for articles
Most Read
- 1
- 2
- 3
- 4
- 5